Research Article - (2015) Volume 23, Issue 5
Department de médecine générale, UFR des sciences de la santé Simone Veil, University Versailles Saint-Quentin en Yvelines.
Montigny le Bretonneux, France
Driat Dorothée
Department de médecine générale, UFR des sciences de la santé Simone Veil, University Versailles Saint-Quentin en Yvelines.
Montigny le Bretonneux, France
De Chefdebien Marine
Department de médecine générale, UFR des sciences de la santé Simone Veil, University Versailles Saint-Quentin en Yvelines.Montigny le Bretonneux, France
François Mathilde
Department de médecine générale, UFR des sciences de la santé Simone Veil, University Versailles Saint-Quentin en Yvelines.
Montigny le Bretonneux, France. CESP, INSERM, Univ. Paris-Sud, UVSQ, Université Paris-Saclay, Villejuif, France
Saunier Audrey
Department de médecine générale, UFR des sciences de la santé Simone Veil, University Versailles Saint-Quentin en Yvelines.
Montigny le Bretonneux, France
Contraception; Intra Uterine Devices; Primary care; France
Around 63% of couples worldwide use a contraceptive method. Among them, 23% choose the Intra-Uterine Device (IUD).[1] In 2005, the IUD was the most popular method of reversible contraception, used by over 160 million women worldwide.[2] The use of IUD is lower among younger women: 9.5% women aged 15 to 24 have chosen the IUD in the U.S. (U.S. Departement of Health and Human Services, 2008), 7.8% in the Netherlands (Centraal Bureau voor de Statistiek, 2008) and 2.6% in Spain (El demostrated daphne, 2009).
In 2004 World Health Organization (WHO) allowed nulliparous women to use IUD.[3] These recommendations are reflected in France in 2004 by the ANAES (National Agency for Accreditation and Evaluation in Health) “IUDs are not only for multiparous women. It is a first-line method of contraception, still considered very effective, with a long duration of action and for which no risk of cancer or cardiovascular disease is established.”[4]
The methods known as long-acting such as the IUD or implants are more effective in real life than pills, patch or ring.[5] Women younger than 21 who use a contraceptive with short duration of action have a risk of unplanned pregnancies twice as important as older ones.
In France, 20 to 23% of women using oral contraceptives have forgotten at least once a pill during the last month of treatment (42% of them during last week), and 92% in the last six months.[6,7] One out of three pregnancies is always described as unintended; two thirds occur with contraception and 60% will end with an abortion.[8,9]
In France, 3.7% of women aged 18 to 24 use an IUD.1 Nulliparous are an important part of them, the first pregnancy average age was 29.9 in France in 2010.8 As the IUD received drug approval for nulliparous women in 2004, what drives them to choose it or not?
Despite clear recommendations of health professionals, IUDs are seldom used by young women. Given the lack of data in France, our objective was to identify the barriers and reluctances for nulliparous women of childbearing age to use IUDs as a contraceptive in primary care.
Study type
A qualitative study was conducted by individual semistructured interviews. Individual interviews were preferred to focus groups for their confidentiality and because they provide information on individual behavior. It creates an intimate promoting expression and allows collecting in-depth information on a topic at the individual level. An interview guide was developed, based on data from the literature and tested by five preliminary interviews (Appendix 1).
The inclusion criteria were: nulliparous women of childbearing age, over 18, French-speaking, and without any mental disease.
Recruitment of participants
The recruitment of participants was carried out on a voluntary basis. It was reasoned on the criteria of age, socio professional category and location of their physician. The enrollment was done in five GPs’ offices, in the Yvelines and the Hauts-de-Seine area (Paris suburb, France). Given the low rate of nulliparous consulting in GP, we extended the recruiting in a second time by "snowball effect".
The number of interviews was not set in advance. The objective was to achieve data saturation, defined in our study as the lack of any new theme raised during three consecutive interviews. Oral consent was sought systematically before each interview both by their attending GP and by the interviewer. The participants were advised that they could interrupt the interview at any time.
Management of the interviews
The interviews were conducted by a resident in general medicine. The interviewer was a woman to enhance the social closeness with patients and chosen to be neutral with the patient. An interview guide that was intentionally undetailed in order to facilitate expression (Appendix 1) was used to guide the interviews.
As the topic is related to the feeling of the patient, a certain intimacy was looked for. We proposed to the patients to realize the interview at their home, for additional confidence and trust related to location. The participants were not incentivized.
Several steps were followed to realize an inductive analysis of thematic content, with category construction based on analysis of the participants’ opinions. The inductive approach is a systematic procedure to analyze qualitative data in which the identified themes are a cluster of meaning-like connected categories. Its primary purpose is to allow research findings to rise from the frequent, dominant or significant themes inherent in raw data.
The interviews were fully recorded and verbatims fully transcribed, with double cross check. Two researchers first coded the results independently, using the software NVivo-9 and conducted a thematic analysis of the data. The verbatim transcriptions were read several times, choosing units of meaning, identifying general themes, categorizing and classifying. The investigators’ triangulation involved two different researchers in the analysis process. The same method was used by each of them to analyze the data. Each evaluator’s findings were compared in order to optimize the data conformity.
The recordings were destroyed after analysis out of respect for medical confidentiality and the private nature of the recorded data.
The study protocol was submitted and approved by the Committee for the Protection of Persons Ile de France IX, dated March 8th, 2012.
Participants’ profile: (Table 1)
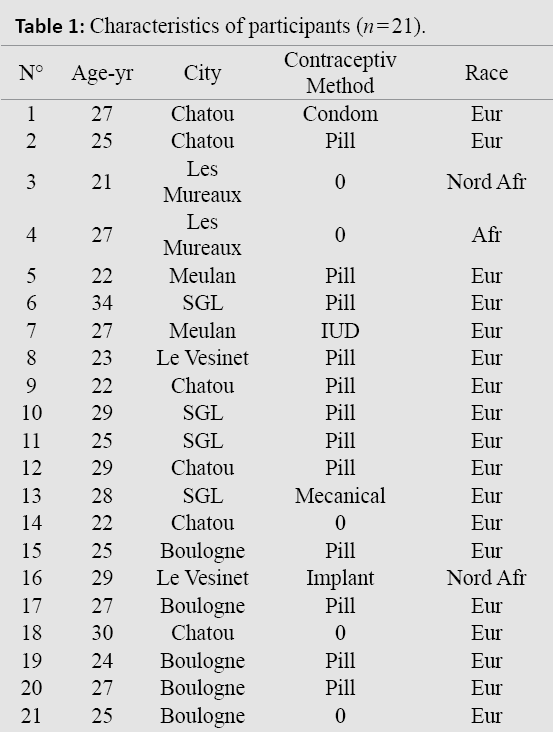
21 interviews were needed to reach data saturation. The interviews ranged from 3 to 20 minutes.
An oft-mentioned lack of information
Interviewed patients emphasized the low media coverage regarding IUD, compared to other forms of contraception, especially compared to estrogen-progestin oral contraceptive.
"I feel that we speak much less of it, compared to the pill." Patient No. 19
Even if they know the word "IUD" and know that it is a contraceptive, women do not visualize the object itself.
Several women ignored the long time effect of IUD, "If we change every three months it becomes restrictive!” Patient No. 18; they imagined an additional constraint of frequent consultations.
Most women kept the idea that the IUD was contraindicated for nulliparous women, either by personal belief or maternal advice. "Finally, my mother always told me ‘no IUD before having your first child’." Patient No.12
The role of their GPs and other health professionals has been recognized by some women as a disincentive to the use of IUD.
The lack of knowledge also concerned anatomical representations: patients were afraid that the IUD might move. Indeed, the location of the IUD was abstract and it generated fears among some women. "I'm afraid it enters the uterus." Patient No. 10
Brakes related to daily concerns
The fear of feeling the IUD, being limited in their daily lives or feeling pain worried patients. "Whether not necessarily pleasant to wear" ... "If ever I feel it, if it’s uncomfortable… ”Patient No. 20 They had the idea of embarrassing circumstances in everyday life as not being able to practice sports, which would condition their choice. "If there are any contraindicated sports or activities” Patient No. 17
And to sexuality
The issue of sexuality was often raised during the interviews. In fact, these women feared that wearing an IUD might prejudice their sexual activity, their personal feelings, or their partners.
"I'm afraid that during an intercourse, it can cause ... It can be quite embarrassing to feel the IUD itself" Patient No. 10
Brakes and psycho-cultural reluctance
The fear of long-term contraception was mentioned several times. It corresponded to the refusal of some form of commitment to a period of life still not stable, and also the need for "freedom" in the initiation and discontinuation of contraception. The women interviewed wanted to control their fertility. In particular, the participants compared the IUD to "the pill" in terms of ease of starting and ending contraception. "It really matters with the long term, unlike oral contraceptives that can be stopped just like that.” Patient No. 02
Amenorrhea was narrated as a side effect. Women saw it as a disruption of the hormonal cycle. They saw in the absence of bleeding a significant brake on the use of IUDs.
Participants evoked doubts about the effectiveness of contraception. "I’m afraid that having an IUD would increase the risk of pregnancy" Patient No. 08 “not reliable at a hundred percent” Patient No 18.
The IUD was seen by women as an abortive contraceptive method. By psychological or sociocultural reluctance, this possible action has been quoted several times. "From my knowledge at school IUD destroys the embryo, I mean, it takes place pretty far in the conception process whereas the pill, I would say, prevents the formation at the level of hormones, at an earlier stage. ” Patient No. 14
Infectious risks
Some patients quoted the risk of pelvic inflammatory disease. “Infection may happen” Patient No. 05.
Influence on fertility
In the idea of future pregnancies, women wanted to ensure their fertility, and they imputed a deleterious role to devices. "The idea of having something in my body... I don’t know, I haven’t studied the issue, but compared to everything we hear, having a metal component and foreign-body uh ... maybe it can be harmful to the body of a woman” Patient No. 17
The IUD is seen as a permanent method of contraception. The women interviewed believed that the IUD was a contraceptive method for women who don’t want any more children and therefore cannot return to fertility. In the absence of initial pregnancies they were not aware of their fertility and feared sterility.
"The fear of um ... not really being able to have any more children afterwards" Patient No. 04
Additionnaly, by its french-name ”stérilet”, IUDs refers to connotations of sterility. « the word doesn’t really scare me, but after, when you think a little more it’s true that it reminds that word: sterile.” Patient No12
Main contributions of the study
This is the first study to directly query, in primary care, French nulliparous women of childbearing age, on their brakes to IUD use. Our results show principally an oft-mentioned lack of information about IUD and brakes related to daily concerns, infectious risks and fears about influence on fertility.
Methodological limitations of qualitative studies lead us to interpret our results cautiously. Despite a strong attachment to methodology and study rules, we can state some bias. The recruitment of patients was carried out on a voluntary basis, initially from all patients GPs, and then by “snowball effect”. This selection has recruited young women interested in contraception and it doesn’t enable the findings to be generalized. However, the aim of this qualitative study was to get a better insight of the barriers coming from patients themselves towards the use of IUD, while avoiding potential subjective bias of the researchers.
Comparison of our results with literature data
Concerning the lack of information, our results seem consistent to those of a study conducted in the United States on for all the adolescents and young women (nulli- or multiparous). [10-13] In this study, fewer than half (45%) of participants had heard about the IUD. Consistently to our work, this study also mentioned the fear of pain during insertion, the fear of having something in the body, the requirement of a health professional for installation and removal, and finally the fear of side effects as brakes for the use of IUD. Concerning sides effects, a Canadian work identified infectious risks and influence on fertility as specially feared by nulliparous women.[14] However, daily concerns were not mentioned as they appear in our study.
Concerning the effectiveness of the contraceptive IUD, the average of unwanted pregnancy (Pearl Index) is 0.6 per year per 100 women using copper IUDs (0.1 Levonorgestrel IUDs.15 However, the Pearl Index requires the optimal use of contraception. The World Health Organization (WHO) reviewed the classification of "current" use criteria (including the notions of forgetting oral contraceptive or condom breakage for example). According to this classification the IUD has a revised Pearl Index of 0.8 pregnancies per 100 women. The efficacy of oral estrogen-progestin in common use is lower with a revised Pearl index of 8 according to WHO .[16,17]
For the risk of infection, the IPPF (International Planned Parenthood Federation) has recently calculated that "when a woman has undergone appropriate screening, it poses little risk of contracting Sexually Transmitted Infections and when the IUD is inserted by using a correct technique, the risk of high genital inflammation exceeds hardly 1 for 1 000”.18
The IUD seems to cause little or no increased risk of infertility in women who are at low risk of infection.19 Shortterm (less than 42 months) use of IUD even allowed a return to fertility more favorable than that observed at the cessation of oral contraceptives on the same period.[20]
Surprisingly, no woman mentioned the risk of ectopic pregnancy during the interviews whereas this risk was often quoted in French medical schools ten years ago. According to a recent meta-analysis, interviewed women were right not to fear this risk. This analysis find that ectopic pregnancy were more common in pregnant women without than with IUD.[20]
Another study described the safety of the IUD and its complications. There was no significant difference in complications between nulliparous and parous women. However, one third of the women had the IUD removed within the first year after insertion. Menstrual problems were frequent and the main reason for IUD removal, but there was no significant difference between nulliparous and parous women. [21] Concerning daily concerns, only one Canadian study showed that the experience of the IUD insertion by nulliparous women was tolerable, even though most of women reported discomfort, such as cramping, during insertion of the IUD or post insertion. In the same time, the women interviewed said that quality of life since insertion had been positive.[22]
On the basis of our results, further quantitative studies can now be considered to quantify and rank the different factors according to their importance. Further research could be done about daily concerns which appear to be a major brake to IUD use among interviewed women.
INPES, Contraception : Les Françaises utilisent-elles un contraceptif adapté à leur mode de vie ? Dossier de Presse, October 2011 ; 4-8