Research Article - (2022) Volume 30, Issue 3
Received: 02-Mar-2022, Manuscript No. ipqpc-22-12989; Editor assigned: 04-Mar-2022, Pre QC No. ipqpc-22-12989(QC); Reviewed: 18-Mar-2022, QC No. ipqpc-22-12989; Revised: 23-Mar-2022, Manuscript No. ipqpc-22-12989(R); Published: 30-Mar-2022, DOI: 10.36648/1479-1072.22.30.24-30
The persistent COVID-19 pandemic caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has led to high morbidity and mortality worldwide [1], which has prompted emergency use of the authorized vaccine to combat SARS-CoV-2 infection. Currently, mRNA, adenoviral vector as well as inactivated whole virus vaccines are now in use widespread [2].
Preliminary studies have shown the safety and efficacy of various vaccines in multiple chronic liver diseases (CLD). In detail, BBIPCorV has been proven to induce a comparable immune response in patients with nonalcoholic fatty liver disease. In addition, patients with chronic hepatitis B virus infection also showed robust immunogenicity and well tolerated during BBIP-CorV/CoronaVac vaccination. However, another prospective study from multicenter revealed that patients with CLD, including hepatitis B, hepatitis C, NAFLD, alcoholic liver disease, autoimmune hepatitis, primary biliary cholangitis, and primary sclerosing cholangitis, had lower immunologic response to SARS-CoV-2 vaccines than healthy population [2]. Despite inconsistence immunogenicity after vaccination in patients with various chronic liver diseases, evidence to date has been lacking on the efficacy of vaccination in patients with metabolic associated fatty liver disease (MAFLD), which is the most common chronic liver disease, affecting about a quarter of the world’s adult population [3,4]. Besides, regarding the persistence of vaccine decline even further over time in health adults who have completed a primary vaccination series, and booster dose administered cloud effectively recalled specific immune response to SARS-CoV-2 [5], and the immune response after vaccination in MAFLD population remains not fully understood. Hence, it seems urgent to explore immunogenicity after vaccination in patients with MAFLD [6,7].
COVID-19 infection was reported to be associated with liver injury and disease progression in MAFLD patients [8]. Besides, concurrent MAFLD was independent risk factor of ALT elevation in COVID-19 patients [9]. Most of the liver injury was mild, mainly characterized by elevated alanine aminotransferase (ALT), and about 33.2% of patients had sustained abnormal liver function during the hospitalization [10]. Considering the deterioration of liver function in MAFLD patients with SARS-CoV-2 infection, monitoring of the disease progression, especially liver function, is a critical component of disease management throughout COVID-19 vaccination. Therefore, prospective longitudinal research was designed to demonstrate the safety, efficacy, and disease flares of SARS-CoV-2 vaccination in patients with MAFLD.
Study Design and Participants
We performed a prospective, observational cohort study that recruited adults (>18 years) receiving SARS-CoV-2 vaccination between 11 January 2021 to 4 February 2021 at the affiliated hospital of Hangzhou Normal University. All participants received two doses of an inactivated vaccine against SARS-CoV-2 (CoronaVac, 0.5 mL/dose, Sinovac life science, Beijing, China) with a 28 day interval. Hepatic steatosis was defined as a controlled attenuation parameter measurement of 248 dB/m or more [11,12], MAFLD diagnosed by hepatic steatosis plus any of the following three metabolic disorders according to the definition proposed by the international expert group [13]: (1) overweight/obesity (≥ 23 kg/m2); (2) type 2 diabetes mellitus or (3) metabolic dysregulation. Metabolic dysregulation was defined as the presence of at least two of the following metabolic risk abnormalities: (1) Waist circumference ≥ 90/80 cm in men and women; 2) Blood Pressure ≥ 130/85 mmHg or use of antihypertensive medications; 3) Triglyceride (TG) ≥ 150 mg/dL or use of lipid lowing medications; 4) HDL-cholesterol (HDL-c) <40/50 mg/dL for male and female or use of lipid lowing medications; 5) prediabetes (fasting glucose levels 100-125 mg/ dL, 2 h glucose levels 140-199 mg/dL or HbA1c 5.7%-6.4%; 6) homeostatic model assessment of insulin resistance (HOMA-IR) ≥ 2.5 [3]. In addition, we included normal weight recipients without hepatic steatosis or diabetes as non-MAFLD participants. This study was approved by the local Hospital Ethics Committee (2021(E2)- KS-049) and written informed consent was obtained from patients involved before enrolment when data were collected. This trial has been registered in Chinese ClinicalTrials.gov (ChiCTR2100042717).
Procedures
Fasting blood samples were captured before vaccination (D0), 28 days after the first dose vaccination (D28), 28 days after the second dose vaccination (D57), and 180 days after the first vaccine dose (D180). Telephone consultations evaluated reactogenicity and safety of each recipient within 7 days after each dose. Adverse events were graded according to the following scale: grade 1 (mild; does not interfere with activity); grade 2 (moderate; interferes with activity), grade 3 (severe; prevents daily activity), and grade 4 (potentially life threatening; emergency department visit or hospital admission) [14]. Seroreactivity and biochemical indicators were detected at each visit. Neutralizing antibodies (Nab) to the receptor binding domain (RBD) of SARS-CoV-2 spike protein was detected by iFlash 2019-nCoV Nab assay (SHENZHEN YHLO BIOTECH CO., LTD, Shenzhen, China, Cat#C86109), which is a paramagnetic particle chemiluminescent immunoassay (CLIA) for the qualitative detection of SARS-CoV-2 Nab in human serum and plasma using the automated iFlash immunoassay system, and the cut off value of 10.00 AU/mL for the antibody [14]. IgG to SARS-COV-2 spike specific were detected by magnetic particle chemiluminescence immunoassay using SARS-CoV-2 IgG detection kit (Beijing Hotgen Biotech Co., Ltd.). The cut off was set as 1.00 Au/ml according to the manufacturer’s guidelines.
Statistical Analysis
All participants with available data were included. Statistics were computed in IBM SPSS Statistics 26 (Armonk, NY: IBM Corp). The significance threshold for p values was less than 0.05 after correction for multiple comparisons. We used the Pearson χ² test or Fisher’s exact test for the analysis of categorical outcomes. We calculated Geometric Mean Titers (GMT) and corresponding IQR of the log-transformed antibody titre then used the t-test method to compare the log-transformed antibody titre. Repeated measures ANCOVA, as implemented under the mixed model [15], was applied with change from baseline as the dependent variable, group, time, and the group by time interaction as independent variables. Age, sex, BMI, and hypertension were included as covariates. The approximate normality of each outcome and the change score of the outcome was confirmed by examination. Logistic regression analysis was used to investigate the generation and durability of Nab at D57 and D180 with various baseline indicators, respectively.
Totally, 164 subjects without a history of the SARS-CoV-2 infection were screened in our research and divided into MAFLD group and non-MAFLD group, comprising 50 MAFLD patients and 114 non-MAFLD participants, respectively. The mean age of the MAFLD group was 42.10 (9.87), and 37.98 (11.8) of the non-MAFLD group, MAFLD group have higher BMI and waist circumference when compared with non-MAFLD group (p<0.05). In addition, there were significant differences in multiple biochemical indexes between two groups, including HDL-c, TG, alanine aminotransferase (ALT), aspartate aminotransferase (AST), uric acid (UA), high-sensitive C reactive protein (hs-CRP), and Homeostasis model assessment insulin resistance (HOMA-IR). The clinical characteristics of study participants were summarized in Table 1.
Table 1. Participants baseline characteristics, comorbidities in two groups.
| Characteristics | MAFLD group (N=50) | non-MAFLD group (N=114) | p |
|---|---|---|---|
| Age (years) | 42.1 (9.87) | 37.98 (11.8) | 0.023 |
| Sex (male/female) | 30/20 | 29/85 | <0.001 |
| Body mass index, BMI (kg/m2) | 26.84 (3.28) | 23.07 (3.26) | <0.001 |
| Waist circumference (cm) | 92.22 (10.29) | 79.75 (8.93) | <0.001 |
| Controlled attenuation parameter, CAP (dB/m) a | 300.72 (36.87) | 206.66 (38.45) | <0.001 |
| Liver stiffness measurement, LSM (kPa) | 5.66 (2) | 4.41 (1.06) | <0.001 |
| NAFLD fibrosis score, NFS | -3.19 (0.22) | -3.17 (0.2) | 0.687 |
| Fibrosis-4 index, FIB4 | 0.85 (0.4) | 0.79 (0.42) | 0.463 |
| Total bilirubin (μmol/L) | 19.57 (7.66) | 19.83 (6.04) | 0.811 |
| Albumin (g/L) | 2.99 (2.9) | 1.5 (0.75) | 0.001 |
| Alanine aminotransferase, ALT (U/L) | 32.27 (24.64) | 15.38 (9.11) | <0.001 |
| Aspartate aminotransferase, AST (U/L) | 25.43 (11.51) | 18.61 (5.94) | <0.001 |
| Alkaline phosphatase, ALP (U/L) | 72.96 (18.98) | 64.54 (19.69) | 0.012 |
| g-glutamyl transpeptidase, GGT (U/L) | 34.78 (28.3) | 19.94 (14.07) | 0.001 |
| LDL-cholesterol, LDL-c (mmol/L) | 3.33 (0.78) | 3.02 (0.78) | 0.019 |
| HDL-cholesterol, HDL-c (mmol/L) | 1.17 (0.22) | 1.43 (0.33) | <0.001 |
| Total cholesterol, TC (mmol/L) | 5.16 (0.91) | 4.86 (0.98) | 0.065 |
| Triglyceride, TG (mmol/L) | 1.44 (0.74) | 0.86 (0.38) | <0.001 |
| Glucose, Glu (mmol/L) | 4.32 (1.64) | 3.92 (0.76) | 0.1 |
| HOMA-IR | 2.982 (2.99) | 1.546 (0.783) | 0.002 |
| Creatinine (μmol/L) | 64.44 (14.36) | 60.09 (31.28) | 0.349 |
| Uric Acid, UA (μmol/L) | 363.12 (101.43) | 292.07 (81.93) | <0.001 |
| hs-CRP (mg/L) | 48.52 (2.73) | 48.12 (2.28) | 0.511 |
| Leukocyte count (109/L) | 6.83 (1.54) | 6.05 (1.38) | 0.002 |
| Platelets count (109/L) | 253.22 (56.24) | 251.49 (59.95) | 0.863 |
| Red blood cell count (109/L) | 5.08 (0.51) | 4.66 (0.62) | <0.001 |
| Lymphocytes (109/L) | 2.33 (0.56) | 2.02 (0.58) | 0.001 |
| hemoglobin (g/L) | 150.62 (17.7) | 138.78 (19.62) | <0.001 |
| Comorbidity, N (%) | |||
| Hypertension | 28 | 27 | <0.001 |
| Diabetes | 5 | 2 | 0.028 |
| Results are expressed as mean (SD) / count (%), a represent the number of MAFLD patients diagnosed by CAP were 46. Pearson χ2 test or Fisher’s exact test were used to analyze the categorical outcomes and t-test for continuous outcomes. hs-CRP represents high-sensitivity C-reactive protein, HOMA-IR represents Homeostasis model assessment insulin resistance. Hypertension was defined as systolic blood pressure ≥130 or diastolic blood pressure≥85 mmHg. | |||
The overall incidence of adverse reactions was 32 (20%) of 164 participants within 28 days after the first dose vaccination, 9 (18%) in the MAFLD group, and 23 (20.2%) in the non-MAFLD group, with no significant difference between the two groups. All adverse reactions were mild and self-limiting. Reported adverse events were graded according to China National Medical Products Administration guidelines [14]. The most common symptom was injection site pain, which was reported by 5 (10%) participants in the MAFLD group, 15 (13.2%) in the non-MAFLD group, followed by fatigue (4%), dizziness (2.6%). Furthermore, there was still no significant difference in the overall incidence of adverse events between two groups within 28 days after vaccinations, which was similar to the results performed in the phase 2 trial of CoronaVac vaccine [2] (Table S1).
Immunogenicity
All individuals were assayed for anti-SARS-CoV-2 spike IgG responses and neutralizing antibodies to the RBD of SARS-CoV-2 Spike Protein. At baseline, none of the participants had any detectable neutralizing antibodies to live SARS-CoV-2. The seroconversion rates of neutralizing antibodies were 16% (8/50) in MAFLD group (Log10 GMT: median 0.783 [IQR: 0.719-0.971]) and 22% (25/114) in non-MAFLD group (0.818 [0.718-0.989]) on 28 days after the first dose vaccination (Day 28). Furthermore, seroconversion rates were upregulated to 82% (41/50) in the MAFLD group (1.206 [1.053–1.467]) and 90% (103/114) in non-MAFLD group (1.329 [1.131-1.439] on 28 days after the second dose vaccination (Day 57), respectively. However, there were remaining 38% (19/50) MAFLD patients (0.928 [0.773-1.057] and 23% (23/96) non-MAFLD participants (0.907 [0.810-1.009]) kept seropositive on day 180. In addition, the seroconversion rates of spike specific IgG were 62% (31/50) in MAFLD group (Log10 GMT: median 0.159 [IQR: -0.203, 0.730], 74% (65/114) in non-MAFLD group (0.239 [-0.382, 0.843]) on 28 days after the first dose, and 100% in both MAFLD group (1.468 [1.054, 1.928]) and non-MAFLD group (1.643 [1.307, 1.895]) on 28 days after the second dose vaccination. By day 180, seroconversion rates were downregulated to 94% in MAFLD group (0.851 [0.534, 1.181] and 98% in non-MAFLD group (0.858 [0.559 1.152]) (Figure 1, Table S2).
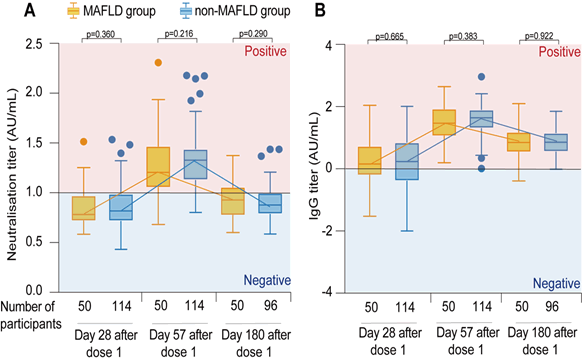
Figure 1: Serological response to SARS-CoV-2 vaccine. Antibody titres of neutralizing antibodies (A) and RBD-specific IgG (B) to live SARS-CoV-2 at different timepoints after vaccination. The horizontal line represents the threshold of specific response. Short bars represent the mean values of titres. Sample comparisons tested by Mann-Whitney U and no significant differences. Line chart represents production and regression of neutralizing antibody and spike-specific IgG (C,F). Ratio of Day 57 to Day 28 represents the production of neutralizing antibody (D) and spike-specific IgG (G) between the two groups, Ratio of Day 180 to Day57 represents the regression of neutralizing antibody (E) and spike-specific IgG (H).
Changes of Biochemical Indicators
Overall, there was no difference between the two groups in the majority of the absolute value changes of biochemical indicators, such as ALT, AST, γ-glutamyl transpeptidase (GGT), HDL-cholesterol, LDL-cholesterol, total cholesterol, triglyceride, glucose, HOMA-IR, UA, and creatinine after adjusting age, sex, BMI, and hypertension on day 28, day 57, day 180. Besides, there was also no difference changes in the majority of biochemical indicators, especially liver function indicators (ALT, AST, GGT) on day 28, day 57, day 180 in patients with MAFLD (Figures 2 and 3, Table S3).
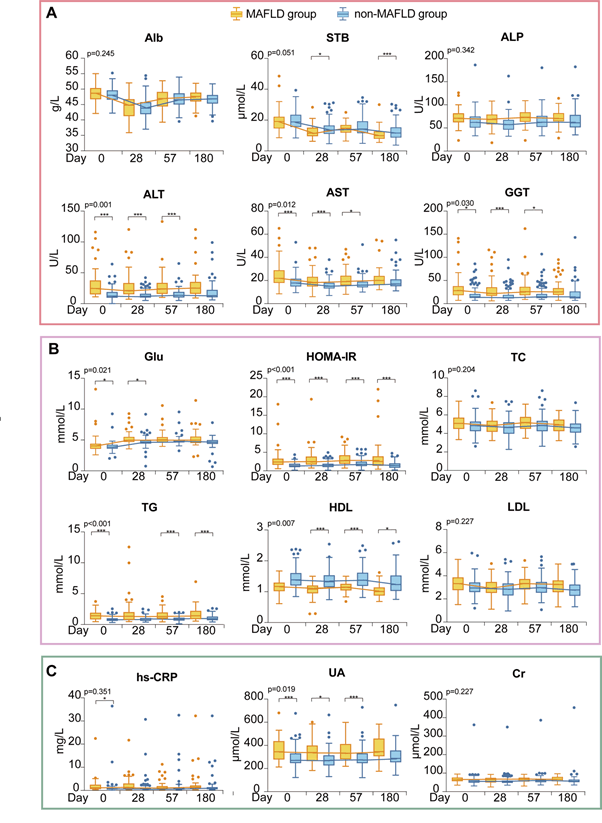
Figure 2: Dynamic changes of biochemical indicators at different time points. (A) Changes of liver function at four assessments. (B) Changes of blood lipid and glucose at four assessments. (C) Changes of renal function at different timepoints. Data were shown as median (IQR). Comparison of the dynamic change of biochemical indicators between the MAFLD group and the non-MAFLD group at different time points by ANCOVA repeated measurement methods after adjusted age, sex, and BMI. The difference between two groups at each timepoints were calculated by t-test. Alb, Albumin; STB, total bilirubin; hs-CRP, high-sensitive C-reactive protein; ALT, Alanine aminotransferase; AST, Aspartate aminotransferase; GGT, γ-glutamyl transpeptidase; ALP, Alkaline phosphatase; Glu, glucose; HOMA-IR, Homeostasis model assessment insulin resistance; TC, total cholesterol; TG, triglyceride; HDL-c, HDL-cholesterol; LDL-c, LDL-cholesterol; UA, uric acids; Cr, creatine. P value shown at the left upper of each indicator was represents the difference between inter-groups. *p<0.05. **p<0.01,***p<0.001.
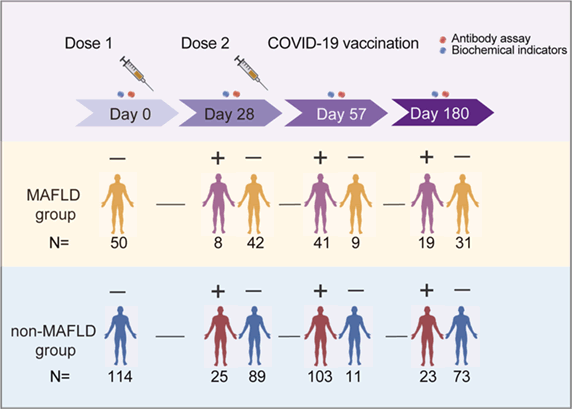
Figure 3: Flow diagram of included participants in our study.
Factors Associated with Seropositive of Neutralizing Antibody on 57 and 180 Days
As shown in Table 2, age, waist, and BMI were significantly associated with seropositive of neutralizing antibody on 57 days by univariate analyses. When these variables were included in the multivariate logistic regression models, we identified that the most parsimonious optimization model prediction only included age and waist, which meant that the odds of seropositive of neutralizing antibody at 57 days were higher in those who with older age (aOR: 0.039, 95% CI 0.900-0.997) and higher waist circumference (aOR: 0.949, 95% CI: 0.906-0.994). Besides, red blood cell and lymphocyte counts were significantly associated with the persistence of Nab on day 180 after adjusted covariates by using multivariate logistic regression method (Table 2).
Table 2. Factors associated with seropositive of neutralizing antibody on 57,180 days, respectively.
| Characteristics | D57 | D180 | ||||||
|---|---|---|---|---|---|---|---|---|
| Univariable analysis OR (95% CI) | p | Multivariable analysis aOR* (95% CI) | p | Univariable analysis OR (95% CI) | p | Multivariable analysis aOR** (95% CI) | p | |
| Age | 0.938 (0.159, 1.054) | 0.008 | 0.039 (0.900, 0.997) | 0.039 | 0.984 (0.951,1.019) | 0.364 | ||
| Sex (male) | 0.409 (0.159, 1.054) | 0.064 | 2.045 (0.981,4.265) | 0.056 | ||||
| Waist | 0.943 (0.904, 0.984) | 0.006 | 0.949 (0.906, 0.994) | 0.027 | 0.995 (0.963, 1.028) | 0.76 | ||
| CAP | 0.998 (0.989, 1.006) | 0.589 | 1.006 (0.999,1.013) | 0.074 | ||||
| LSM | 0.882 (0.664, 1.170) | 0.383 | 1.299 (1.019,1.656) | 0.035 | ||||
| BMI | 0.887 (0.791, 0.993) | 0.038 | 0.981 (0.891, 1.081) | 0.703 | ||||
| ALT | 1.010 (0.977, 1.043) | 0.568 | 1.024 (1.003,1.045) | 0.025 | ||||
| AST | 1.009 (0.952, 1.069) | 0.769 | 1.051 (1.007,1.096) | 0.022 | ||||
| ALP | 0.996 (0.974, 1.019) | 0.737 | 1.010 (0.992, 1.027) | 0.275 | ||||
| CRP | 1.145 (0.938, 1.399) | 0.183 | 1.151 (0.989, 1.340) | 0.068 | ||||
| Glu | 1.065 (0.663, 1.710) | 0.795 | 0.867 (0.595, 1.264) | 0.459 | ||||
| HOMA-IR | 0.903 (0.746, 1.093) | 0.295 | 1.117 (0.931, 1.339) | 0.233 | ||||
| WBC | 0.921 (0.671, 1.265) | 0.613 | 1.324 (1.025,1.710) | 0.032 | ||||
| RBC | 0.733 (0.309, 1.736) | 0.48 | 3.461 (1.634,7.332) | 0.001 | 2.746 (1.212, 6.223) | 0.016 | ||
| lymphocytes | 0.931 (0.421, 2.059) | 0.861 | 2.758 (1.397,5.442) | 0.003 | 2.377 (1.150, 4.914) | 0.019 | ||
| hemoglobin | 0.996 (0.971, 1.021) | 0.751 | 1.025 (1.003,1.048) | 0.028 | ||||
| *Adjusting for age, waist, BMI **Adjusting for LSM, ALT, WBC, RBC, lymphocytes, and hemoglobin | ||||||||
Previous studies reported that the incidence of COVID-19 was higher in MAFLD group than in non-MAFLD group [16,17]. In addition, metabolic disorders might also be significant risk factors of hospitalization and severity in COVID-19 patients [18,19]. Therefore, it’s urgently needed to explore the CoronaVac responses in MAFLD patients as those patients may be uniquely susceptible to COVID-19 infection and disease progression. To the best of our knowledge, this is the first prospective report of the safety and immunogenicity of CoronaVac in MAFLD populations. Our study indicated that there was no significant difference in the overall incidence of adverse reactions after two dose vaccinations between two groups, and CoronaVac did not affect the biochemical indicators in MAFLD patients. Furthermore, we detected that age and waist circumference were inversely associated with seropositive of neutralizing antibody on 57 days, red blood cell and lymphocyte counts were significantly associated with the persistence of Nab on 180 days in total recipients.
Similar to the general population [19], side effects related to the CoronaVac in the general population were mild and self-limiting, and the most common symptom was injection site pain, followed by fatigue, dizziness, and diarrhea. No serious adverse events were reported in MAFLD patients. Our results demonstrated that a two dose regimen of 3 ug of inactivated CoronaVac vaccine administered 28 days apart to MAFLD patients was safe and well tolerated. More importantly, we did not find changes of biochemical indicators, especially ALT, AST, GGT, throughout vaccination in MAFLD patients, which means that CoronaVac might not affect the disease status and prove the safety of CoronaVac in chronic liver disease population.
Vaccine immunogenicity and efficacy are broadly assumed to require neutralizing antibodies, which could target the receptor binding domain (RBD) of the spike protein of SARS-CoV-2, then blocking bound to the ACE2 receptor of host cell, thus inhibiting viral infections [20,21]. Strikingly, our results identified that two dose CoronaVac induced neutralizing antibody and spike specific IgG in MAFLD patients were comparable [22]. Similar to the study performed by Wang et al., [23] CoronaVac elicited a high immune response in our cohort in the short term, with 82% vaccine efficacy in MAFLD group at 28 days after two dose vaccinations. However, the GMT of Nab declined to below the positive cutoff titer after 6 months of vaccination in our cohort, which also consistent with the results of Pan et al.’s study using the same vaccine. And this study also found that a third dose vaccination, given at an interval of 6-8 months after the second dose could lead to a significant rebound in antibody levels, which indicating that booster vaccination may be necessary.
On multivariable logistic regression analysis, few variables were associated with seroconversion rates of neutralizing antibodies after vaccination and liver steatosis, abnormal liver function, and elevated BMI were not associated with the poor antibodies responses, which provides encouraging evidence for MAFLD patients, who should be more actively involved in SARS-CoV-2 immunization. However, age and waist circumference were inversely correlated with the seropositive of neutralizing antibody on days 57, red blood cell and lymphocyte counts were significantly associated with the persistence of Nab, which could provide promising predict indicators for neutralizing antibody generation. Nevertheless, we acknowledge the following limitations. First, the sample size of the study is small. Besides, this study does not evaluate T cell responses and the production of memory cells between the two groups and data on immune persistence needs further study. Furthermore, the study lacks a comparison to convalescent samples, especially in the absence of a correlate of protection, but these have been considered in our further research. Despite these limitations, we believe our observations are very important and meaningful. Our study is the first prospective study of COVID-19 vaccine in MAFLD patients to date. It is safe and effective to receive the CoronaVac in MAFLD patients, which does not affect disease status. Therefore, MAFLD patients should be involved in immunization to against SARS-Cov-2 as the highly vulnerable patient population with higher morbidity and mortality risk. However, immune response does not seem to be sustained in the long term, thereby a third dose could be necessary to boost immunity. However, future studies should consider booster doses in those with undetectable and suboptimal antibody responses.
CoronaVac vaccination in MAFLD patients was safe and well tolerated. MAFLD patients showed a similar immune response to health controls.
JP Shi, J Li and L Shao conceived and designed the study, QR Zhu, J Gao, JP Gu, L Shen, J Liu, Y Song, XY Gong, YT Chen, J Liao, YN He, SY Zhang collected data, QR Zhu performed the statistical analysis, QR Zhu, L Shao, J Li interpreted data, QR Zhu and J Li wrote the manuscript. All authors critically reviewed or revised the manuscript and approved the final version of the manuscript.
This work was supported by Project of Key Medical Disciplines of Hangzhou, the Health and Science and Technology Planning Project of Hangzhou municipal Health Commission [grant number: No. A20210205].
JP Shi reports grants from Project of Key Medical Disciplines of Hangzhou for the Department of infectious and Hepatology. QR Zhu reports grants from the Health and Science and Technology Planning Project of Hangzhou municipal Health Commission, during the conduct of the study. All authors declare no competing interests.
The data will be shared on reasonable request to the corresponding author.
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed] [Research gate]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
Citation: Qianru Zhu, jin Gao, Jiaping Gu, Lu Shen, Jing Liu, et al. (2022) Evaluation of Immune Response and Disease Flares in Metabolic-Associated Fatty Liver Disease (MAFLD) Patients Following SARS-CoV-2 Vaccination: A Prospective Study. Qual Prim Care. 30.41801
Copyright: �????�???�??�?�© Qianru Z et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.