Research Paper - (2005) Volume 13, Issue 4
Associate Professor, Division of General Practice, School for Primary, Aboriginal and Rural Health Care, University of Western Australia, Claremont, Australia
Jennifer Freeman PhD
Lecturer in Medical Statistics
Claire Fisher
Medical Student
University of Sheffield, UK
Geoff Schrecker MRCGP
General Practitioner
Michael Gordon MB BS BMedSci
General Practitioner
Gleadless Medical Centre, Sheffield, UK
John Reid MBChB DRCOG FP (Cert)
General Practitioner, Kiveton Park Primary Care Centre, Kiveton Park, Sheffield, UK
Received date: 18 August 2005; Accepted date: 2 November 2005
Introduction The management of hypertension in the older individual is complicated by the need to take into account the effect of the ageing process. However, older hypertensive patients are at higher risk of vascular disease, and therapy may be morecost-effective in this age group. Methods A retrospective review of case notes at two general practices serving over 19 000 patients in the UK. Patients were aged 75 years or older and treated for hypertension for at least one year at the time ofsurvey. The latest recorded blood pressure was used to identify patients who remained hypertensive despite drug treatment. Therapy prescribed, patient preferences recorded, investigations performed, scope for further therapy and documented plans for management were compared. In the second part the general practitioners were asked to explain why some patients were offered more medication than others.Results Three-hundred and twelve records were surveyed. Differences in the management of cases between the two practices were noted. One-hundred and nine patients were prescribed three or more classes of therapy. Asignificantly greater proportionof these cases were prescribed higher doses or additional therapy at their last consultation. Patients who were offered a more ‘active’ approach were thought to be better informed and better advocates for themselves.Discussion Overall the data suggest inconsistency in the management of a group with the same disorder. Contrary to expectations, patients who were already prescribed three or more antihypertensive agents were more likely at their most recent consultation to be offered even higher doses or additional drugs, than those on fewer agents. Subjective biases, faulty generalisations and lost opportunities for reviewing therapy may account for differences in the management of the same patient group. Further research into factors that influence the application of clinical guidelines with reference to the consultation in primary care is warranted.
general practice, guidelines, hypertension
Seventy-six-year-old Joyce Latham presented to the surgery for the third time in six months and waited quietly as her doctor measured her blood pressure and noted the reading on her computer records. ‘Your blood pressure is a little high this morning’, he said.
Hypertension, an asymptomatic condition, usually requires lifelong therapy with multiple prescribed drugs on a convenient dosing schedule.[1,2] The potential for vascular events, a recognised consequence of hypertension, can be reduced to a great extent when treating this disorder in older individuals up to 80 years of age.[3–5] However, when prescribing appropriate therapy for these individuals the physiological effects of ageing and the presence of co-morbid conditions must be taken into account to avoid iatrogenesis. The goal is to control blood pressure without compromising the functional wellbeing of patients.[6] Some experts perceive dangers in prescribing more than one therapeutic agent in the context of advanced age, while others maintain that effective drug therapy need not compromise quality of life.[7,8] In unresponsive cases there is no agreement on when to stop trying to reduce blood pressure, while the patient is able to tolerate yet more therapy.
In a previous cross-sectional survey, we reported that practices in South Yorkshire successfully treated 60% of their older hypertensive patients when using two or more classes of antihypertensive medication over a three-year period.[9] This is a greater proportion than reported in previous studies, which included the generality of patients.[10] However, our earlier audit did not include a review of plans for further care. We have now conducted a detailed review of records for older hypertensive patients, and compared what therapeutic manoeuvres have been performed or have been planned for this cohort, and what practitioners say about the management of hypertension for older patients with reference to specific cases in clinical practice.
Part 1
Part 1 was a retrospective review of case notes in general practice. The project was based at two practices in South Yorkshire serving a moderately deprived community. The characteristics of the practices are outlined in Table 1. A search identified patients coded for hypertension on the practice computer records. The inclusion criteria for the survey were: patient 75 years of age, coded for hypertension on practice computer by April 2005 and diagnosed by April 2004 and most recent systolic blood pressure 150 mmHg and or diastolic blood pressure 90 mmHg. The latter criteria are consistent with the Quality and Outcomes Framework 2004/05 published by the UK National Health Service, Health and Social Care Information Centre.11 The data collected are shown in Box 1.


Part 2
These data were discussed by general practitioners (GPs) and practice nurses at each of the participating practices. Individual patients with sustained hypertension over one year were selected, and their cases presented to the relevant practitioners. The methodology mirrored the structured investigation of clinical incidents as described by the Clinical Risk Unit (CRU) on their website.[13] Practitioners were asked to state the reasons why in individual cases they had chosen to prescribe or withhold therapy. Examples of two contrasting cases were presented for review; those taking only one class of medication, who remained hypertensive but to whomno further therapy was offered or recorded, and those individuals on three or more agents where the dose of the prescribed drugs was altered or new agents added at the last consultation. Comments were invited about what factors were thought to facilitate the management of hypertension and those that make it more difficult. The reasons offered were summarised as those operating at the level of the patient, the practitioner and the primary care team. It was acknowledged that there were also factors that relate to the consultation, the tasks that must be accomplished in that consultation, doctor– patient communication, and where the patient accessed care in relation to their condition, be it a consultation with the GP at the surgery, at home or by attending a nurse-led clinic. A summary of the conclusions from this discussion is presented in Table 6.
Overall management of cases
Three-hundred and twelve eligible patient records were surveyed. This was equivalent to 21% of the list of older patients at each practice, excluding cases diagnosed within the 12 months before the survey. It is estimated that the prevalence of hypertension in the older patients is more than double this number, and that half the patients remain undiagnosed.[14,15] There was a preponderance of female patients. The age of the patients and their blood pressures were broadly similar at both practices (Table 2). In over 85% of cases, the GP had documented no patient preference about the management of their hypertension. Only a few patients had been referred to a hospital clinic. Neither practice was more active in managing cases of sustained hypertension over one year (Table 3). There was scope to alter therapy of 94% of all patients, either by increasing the dose of the current therapy or adding another agent with reference to the British Hypertensive Society guidelines.[12] In particular it may have been possible to improve therapy for all 66 patients who had suffered no side-effects at any time, compared to the rest where further therapeutic options were possible in 92% of cases. The difference of 8% in these proportions was significant with 95% confidence intervals ranging from 0% to12%.
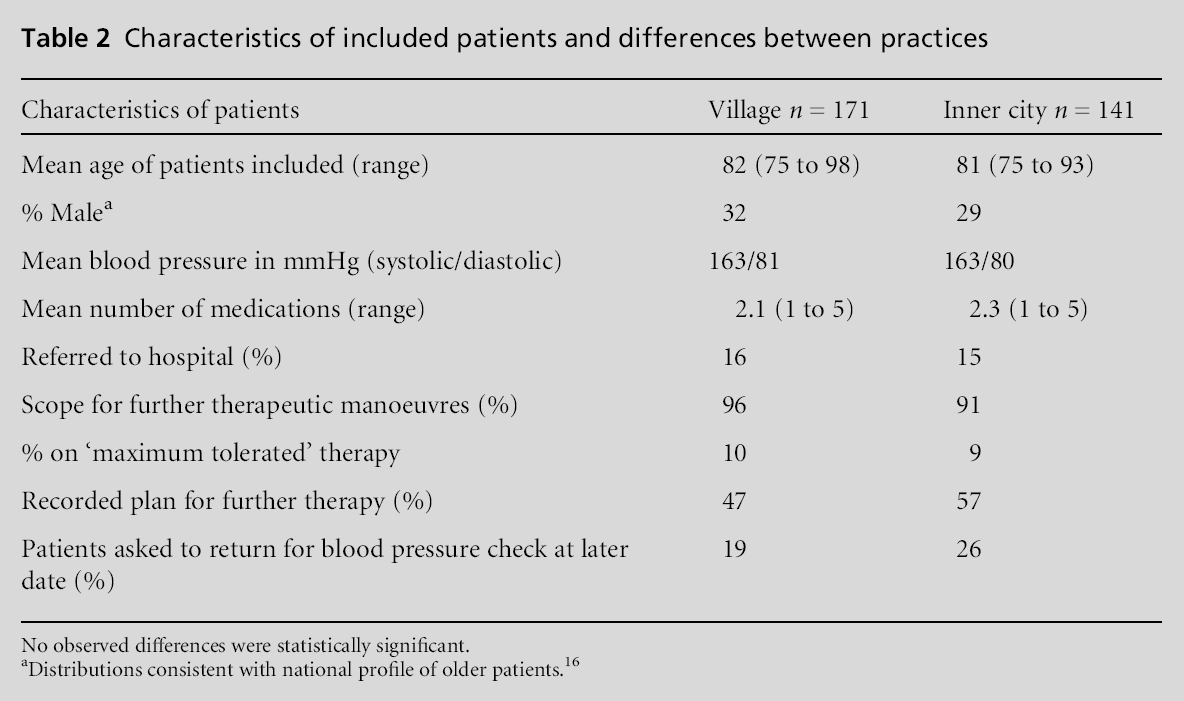
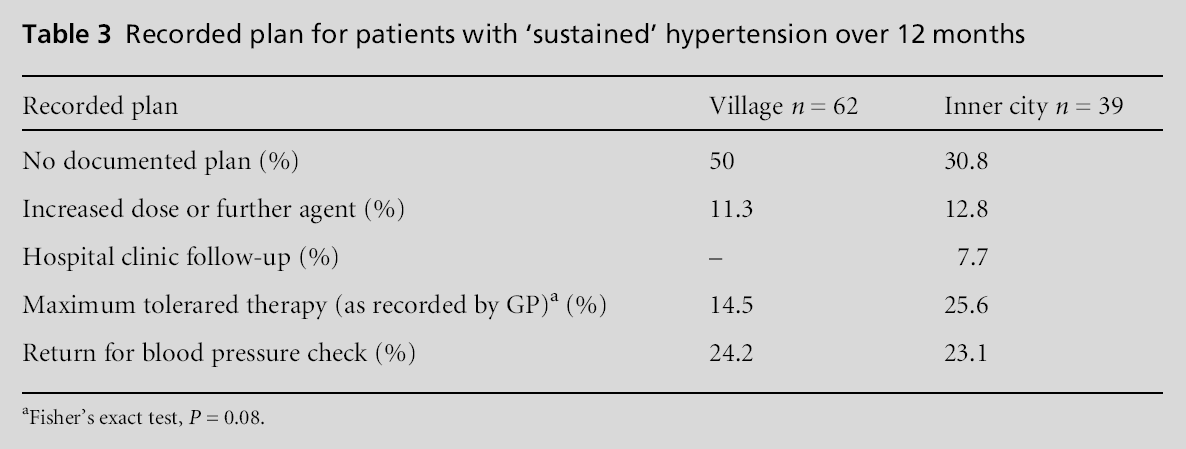
Differences between practices
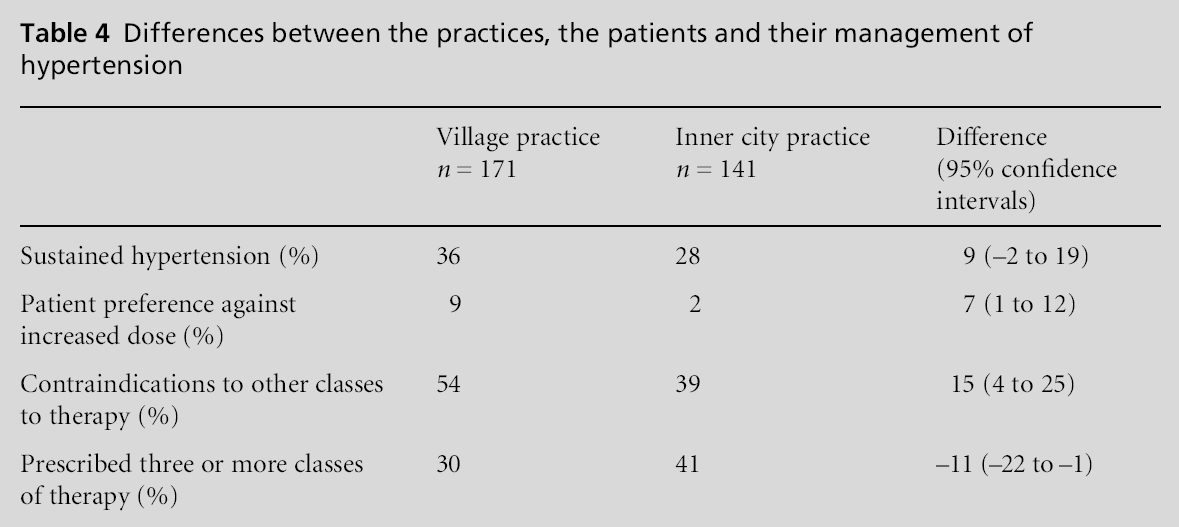
The village practice had a greater percentage of patients with sustained hypertension, and in a greater percentage of their records doctors had documented patient reluctance to accept a higher dose of medication. More patients at the village practice had contraindications to specific classes of therapy, while more patients at the inner-city practice were taking three or more agents. Significant differences between the practices are outlined in Table 4; note the wide confidence intervals with respect to these differences.

Polypharmacy
Sixty-nine per cent of patients were taking more than one class of antihypertensive drug with similar proportions in both practices. This group were neither younger nor more likely to be male than the rest of this cross-sectional sample. Patients who were on three or more classes of therapy (109 cases) were managed more actively with a plan for further therapy or dose change in half of all cases. This was unexpected, as there was equal scope to alter therapy for patients taking fewer antihypertensive agents. Secondly, although diastolic pressures were lower in the group taking more than three agents, these differences were statistically significant, but arguably not clinically significant. Side-effects were not reported as more common in those on multiple agents. Finally, patients taking fewer drugs were no more likely to be recorded as having expressed a preference about their treatment when compared to those on three or more drugs (Table 5).
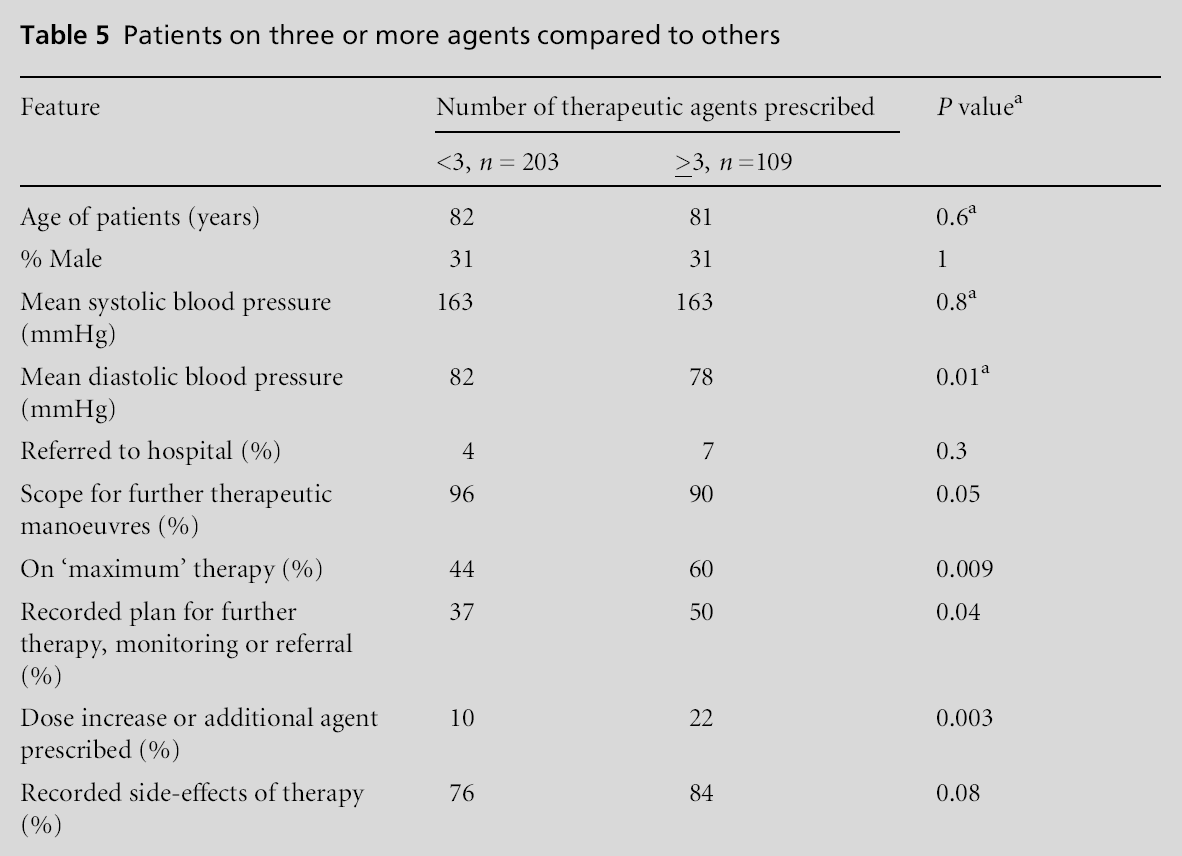
General practitioners’ perspective
Practitioners recognised a variety of factors that impact on planning for patients with hypertension. Short consultations, in which older and frailer patients present multiple symptoms within the context of acute illness, were cited as the principal reason that the patient’s hypertension was not addressed in some cases. However, where patients were able to act as their own advocate and presented at a consultation focused specifically for treatment of hypertension, then a more liberal prescribing policy was facilitated. The involvement of a nurse or hospital clinic was considered likely to improve the patient’s chances of being managed more actively by all concerned. The deliberations are summarised in Table 6.
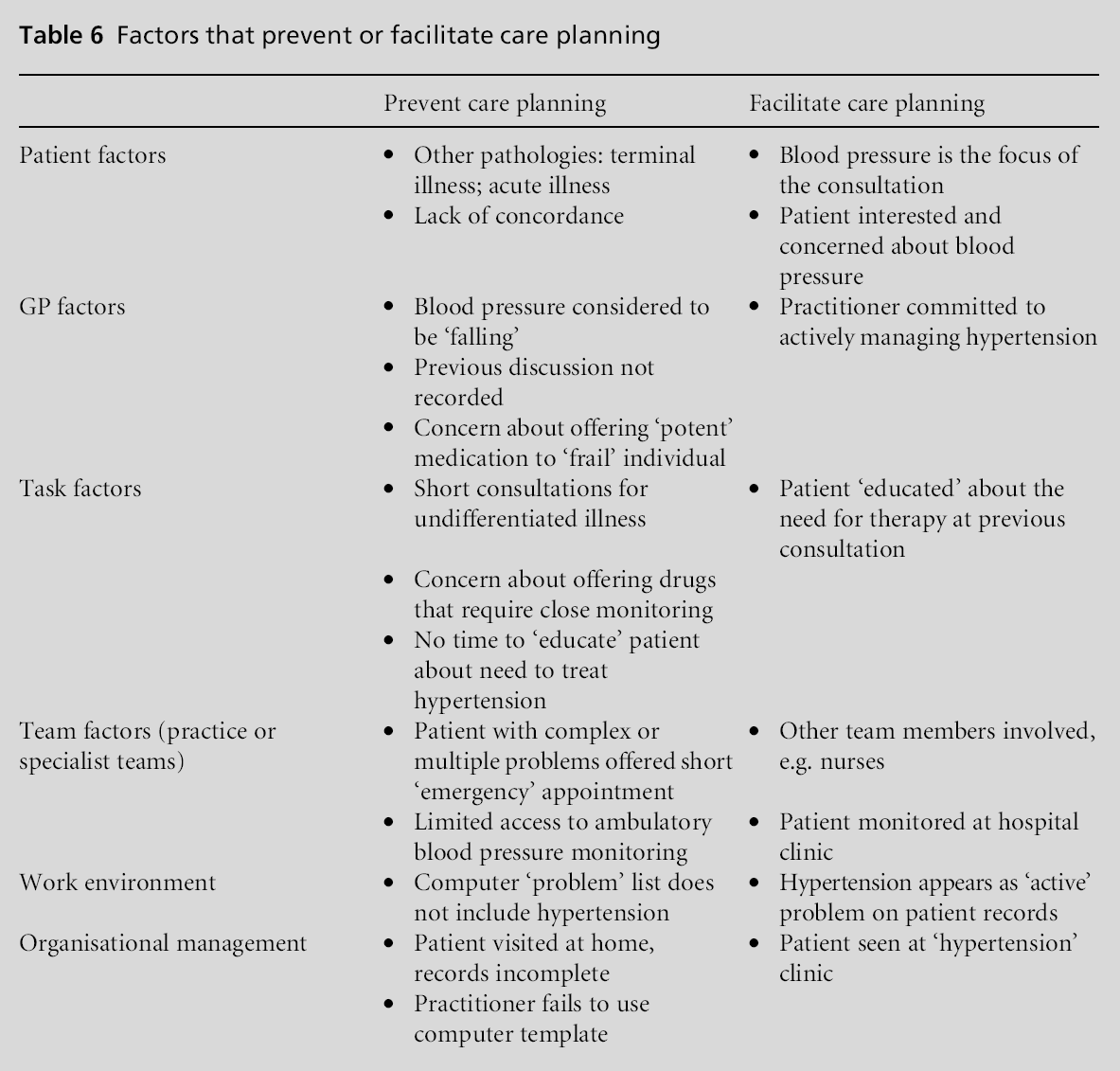
Those patients taking three or more drugs were not distinguished by virtue of a documented patient preference for doctors to prescribe more generously. Nor had those taking fewer drugs experienced documented side-effects on previous occasions. Contrary to expectations, patients who were already prescribed three or more antihypertensive agents were more likely at their most recent consultation to be offered even higher doses or additional drugs, than those on fewer agents. Furthermore a higher proportion of those taking three or more drugs were already considered to be on maximum tolerated therapy.
This survey relies on documentary evidence from patient records. The doctors involved acknowledge that their notes do not offer a comprehensive record of the doctor–patient discussion or the therapeutic plan. The perspective of the patient is absent and we recognise this as a weakness in drawing conclusions about patient care.On the other handwe offer comparisons between practices in very different localities, and report differences in approach to patients, suggesting that the results may be generalisable by virtue of this observed heterogeneity. Such differences are small and characterised by wide confidence intervals. The novelty of our approach is the inclusion of the practitioner perspective focused on specific cases where contrasting treatment was offered within the context of the same healthcare system. The overall impression from the data is inconsistency in approach to the same disorder. UK GPs are now financially rewarded for actively managing patients with hypertension, with higher payments when hypertension is successfully treated.[17] However, these data reflect the findings of others insofar as a substantial number of patients who remained hypertensive were not offered additional therapy.[15]
Both patient and doctor play a critical role in the therapeutic alliance as was highlighted by the respondents in Table 6. Gabbay and le May postulated that many factors influence the practitioner’s response to guidelines.[18] In this context the relevant theoretical framework might be decision-making theory, which offers a rationale for differences in management.[19] It is generally agreed that biases can creep into the decisionmaking process.[20] Therefore the justification for a passive approach offered by the observation that a patient’s blood pressure is ‘falling’ without intervention may be ‘wishful thinking’. ‘Faulty generalisations’ may apply in those cases that are regarded as ‘too frail’ for ‘potent therapy’, especially as all patients were taking at least one therapeutic agent to manage their hypertension and any drug can be ‘potent’ or offered at lower dose. On the other hand, where patients expect to be offered alternative or additional drugs, practitioners might be said to conform to the decisionmaking expectations that the patients have of their medical advisor in this context, i.e. ‘role fulfilment’. Finally, individuals prescribed more than three agents and who continue to be actively managed could be examples of ‘incremental decision making’ and ‘escalating commitment’. Each consultation results in a small step in the process, and perpetuates a series of similar decisions.
Therefore, in theory, and within the limitations of the data presented here, decisions on treatment relate to how and when the patient presents and may be a product of the interaction between the protagonists. We accept that this commentary remains speculative. The next step may be the detailed investigation of individual consultations in which management plans may be subject to guidelines and include practitioner and patient perspective. The challenge is to design a study that does not alter the dynamic or range of the doctor–patient consultation while investigating the application of guidelines. If notable biases are identified, then the appropriate intervention may be fashioned to improve patient care and may be taken into account when developing guidelines.
None.