Patient Perspective - (2009) Volume 17, Issue 4
Chief Executive, National Association for Patient Participation, UK
Received date: 1 July 2009; Accepted date: 8 July 2009
This article brings together research carried out by the National Association for Patient Participation from 2005 to 2009. Its aim was to capture the views of GP surgeries that have patient participation groups (PPGs) as well as those who do not. It also studied the views of PPGs affiliated to the National Association for Patient Participation (NAPP) about their role, their organisation and the support that they require to maximise their success. With the exception of the online, UK-wide members’ survey, the research was carried out through postal surveys sent to more than 4000 English practices in three separate studies. The main results relate to the prevalence of PPGs, their geographical location, their activities, the attitudes of practices towards PPGs (especially those that do not have one) and the future needs of PPGs. PPGs are seen to play an important role in providing the practice with the patient perspective but they are active in several other areas, including health promotion, information provision, influencing commissioning, supporting other patients and fundraising (for their own needs as well as those of the practice). Three central challenges are highlighted, relating to (a) the most successful strategies to promote more PPGs; (b) the importance of support from primary care trusts (or their equivalent organisations); and (c) ways in which PPGs can increase their ability to represent the wider patient perspective. A future research agenda is also proposed that would evaluate the costs and benefits of PPGs across their broad range of activities.
patient participation groups, primary care
The first Patient Participation Groups (PPGs) in the UK were established in 1972. Since then, the model has gradually spread so that 41% of English practices now have a PPG (NHS InformationCentre, 2009, unpub-lished). This paper brings together research undertaken by the National Association for Patient Participation (NAPP) over the past four years. Collectively, it rep-resents the most comprehensive picture ever captured of the activities of PPGs and attitudes towards them.
After a brief generic description of PPGs, this article describes the methods by which data have been obtained from practices and PPGs. It then presents the findings, looking at the prevalence of PPGs, their location and activities, attitudes towards PPGs and reflections on their future development. The closing section considers some of the main themes that have been identified, discussing how to motivate more PPGs and how they might be as effective as possible.
PPGs are groups of volunteer patients, typically based at a single general practitioner (GP) surgery. They evolve to meet particular local needs. Each one is different, free to choose how to organise itself and where to focus its activities. They typically require support from the practice to get started but, over time, they should be run by the patients themselves. It is important that good relations with the practice are retained, so that PPGs can contribute to the partner-ship between practices and their patients.[1] The range of current PPG activities is described later in this article.
From 2004 to 2007, NAPP received three-year Funding from the Department of Health in England to identify areas where patients were able to influence primary care services. That project included a major survey of GP practices (referred to below as the national survey). This started with a pilot phase where one practice in each English primary care trust (PCT) was invited (by post) to fill in the appropriate survey, depending on whether or not they had a PPG. Fifty practices were also contacted by telephone to iron out any problems with the wording of the questions.
The revised surveys were then sent by post to just over 1800 GP surgeries, six in each of the 302 English PCTs that existed at the time. After one reminder letter, exactly 500 completed questionnaires were received, representing a response rate of 28%. The exercise was repeated in 2007, with a further six practices in each of the ‘old’ (since the boundaries had now changed) PCT areas. The response rate, again following one reminder letter, was 29%. In 2005, 78% of the surveys were completed by practice managers, 19% by GPs and 3% by other practice staff.
In 2007, the figures were 89%, 7% and 4%, respect-ively.
In summer 2008, NAPP received further English Department of Health Funding to promote PPGs in 11
PCTs. The PCTs that were invited to participate were chosen in order to achieve a broad geographical spread, as well as contrasting stages of development in the prevalence and dynamism of the PPGs on their patch. Each PCT was invited to collaborate in a survey of its practices (subsequently referred to as the map-ping survey). Seven of these had been completed by June 2009, with 315 replies to 519 requests for infor-mation. This response rate of 61% was helped by reminders that were used in most areas. Eighty-five percent of the surveys were completed by practice managers, 8% by GPs and 7% by other practice staff.
The mapping survey closely resembled the national survey. However, two PCTs preferred to use a modi-fied version based on comments received from prac-tice managers in Oxfordshire who were consulted as part of the process. This led to the inclusion of sections for practices with a dysfunctional PPG and practices where a PPG had disbanded. The numbers of practices fitting these categories were low and so are disregarded in the analysis that follows. The seven PCTs, with the number of practices given in brackets, are Bradford (89), Hillingdon (49), Milton Keynes (27), Notting-hamshire County (103), Oxfordshire (82), Somerset (75) and West Sussex (94).
The third set of results comes from NAPP’s own members’ survey carried out in spring 2009. This was designed as an online survey but hard copies were distributed to affiliates who did not use email. The questions were developed after consultation with the NAPP Board and a sample of nine PPG members who were able to suggest improvements before the survey was distributed. At the time of the survey, NAPP had 410 PPG affiliates and received 135 replies, a response rate of 33%. No chasers were sent to boost this number.
The combined surveys contain a vast amount of detail that cannot adequately be captured here. Instead, areas of particular interest and relevance are identified, focus-ing on the quantitative data rather than the rich free-text comments that have been received.
In the national survey 2005, one in four practices (25%) reported having a PPG. By 2007, this figure had risen to 37%. In the mapping survey 2008/2009, 41% of practices reported having a PPG.
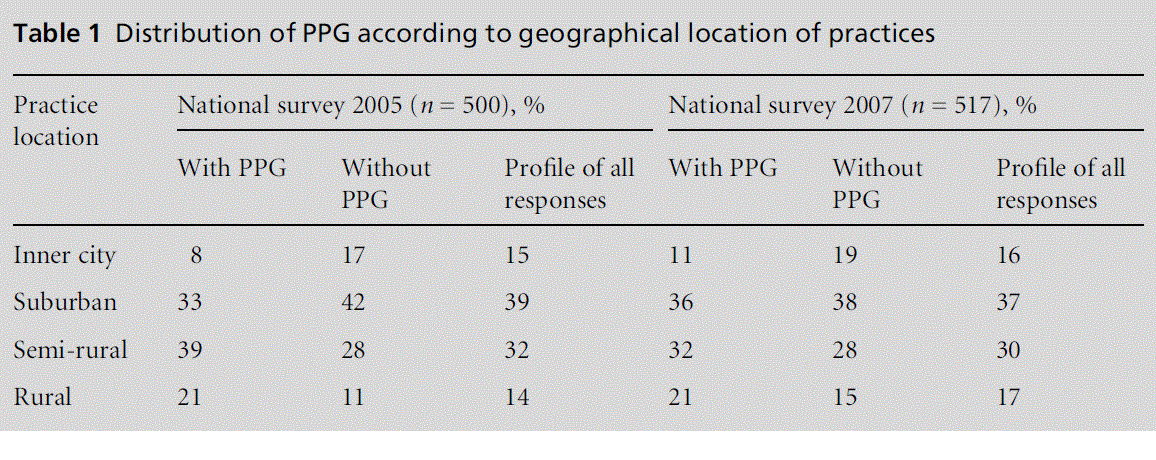
Both the national and the mapping surveys demon-strated that practices in rural areas were considerably more likely than those in suburban settings to have a PPG (see Table 1). Note that percentages in the tables that follow do not always sum to 100 due to rounding errors.
Similar questions were asked about the influence of the PPG with respect to the PCT and the wider NHS. Thirteen percent of practices felt that their PPG was quite or very influential with their PCT in 2005 com-pared to 10% in 2007. Seven percent of respondents to the members’ survey judge themselves to be quite or really influential with ‘the wider NHS’.
In the national and mapping surveys, practices were asked to assess the influence of the PPG ‘in the life of the practice’. In 2005, 44% considered their PPG to be quite or very influential, a figure that fell to 38% in the 2007 survey (when the average age of the PPGs was two years less). The equivalent figure for the mapping survey was 44%. A similar question (‘how influential is the PPG with respect to practice decision making?’) was included in the members’ survey 2009, where 48% of NAPP affiliates considered themselves to be quite (40%) or really (8%) influential ‘with respect to prac-tice decision making’.
The current activities of PPGs, as captured by the mapping exercise, are summarised in Table 2.
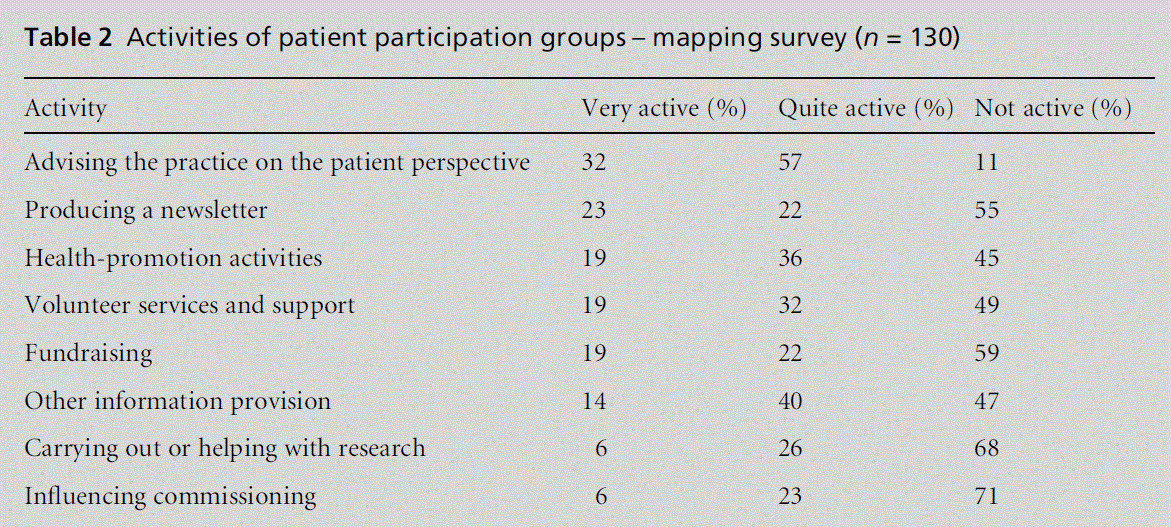
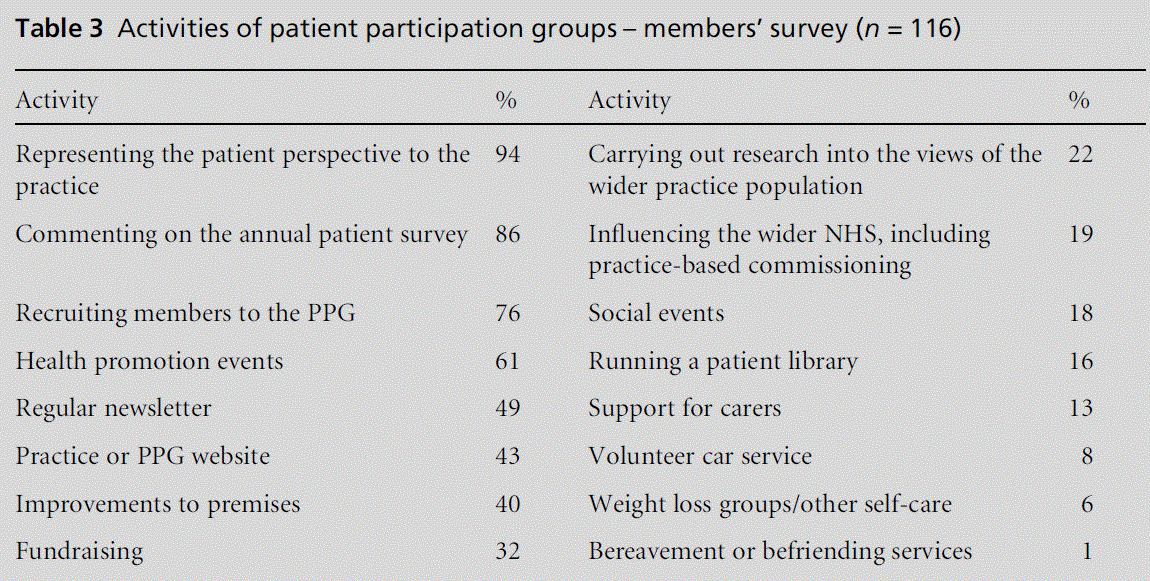
They can be compared with the responses of NAPP affiliates in the members’ survey. Figures are percent-ages that represent the numbers of PPGs who are active in each area (see Table 3).
In 2005, nearly 70% of practices without a PPG had considered setting one up. In 2007, this figure stood at 77%. For the mapping survey (where some work to promote PPGs may already have taken place) the figure was 82%. Why then did practices decide not to go ahead?
In the national survey, respondents were able to offer free-text comments to explain their decision not to proceed. Lack of time was the most commonly cited reason, followed by (in no particular order):
• a feeling that the practice was already close to its patients
• perceived lack of interest among patients
• fear that the wrong patients will be interested
• the difficulties of working with a diverse patient population
• a previous failed attempt at establishing a group.
These responses informed the mapping survey which was able to quantify the significance of these factors as follows:
1 If you have considered setting up a patient partici-pation group, please indicate how significant the following factors are in the practice’s decision not to establish one (see Table 4).
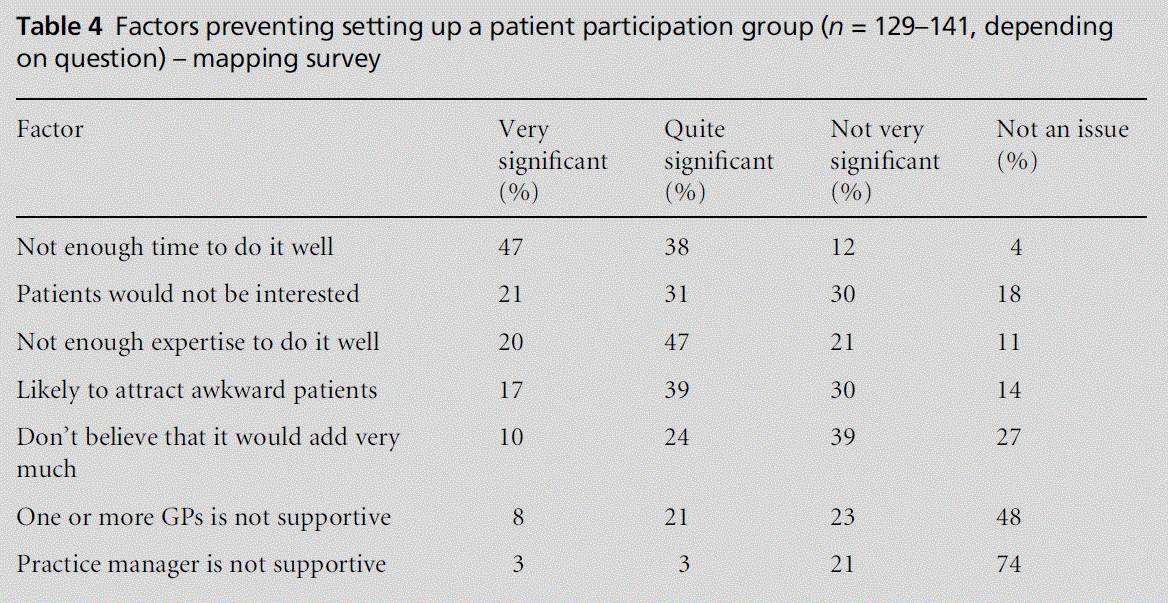
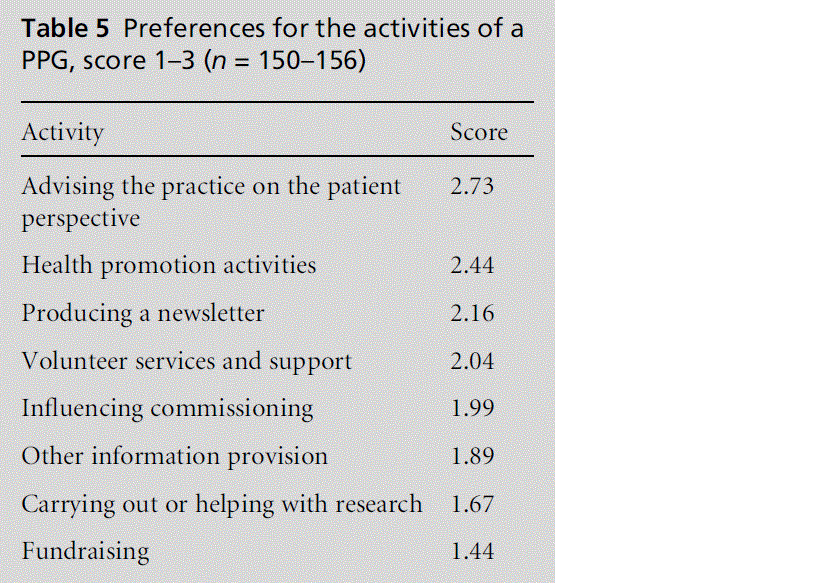
2 Respondents were also asked to state their prefer-ences for the activities of a PPG if one was eventu-ally started at their practice. If three points are scored for a high priority, two for a medium priority and one for a low priority, their ratings were as shown in Table 5.
NAPP members rated the usefulness of ten factors in helping their PPG to achieve its full potential (on a four-point scale where one is not useful and four is very useful) (see Table 6).

Practices with PPGs addressed a similar question as part of the mapping exercise that asked ‘how import-ant would you rate each of the following in helping the PPG to achieve its true potential?’ (scored on a five-point scale; see Table 7).

We close with two areas covered by the members’ survey. First, only 25% of PPGs reported receiving any help from their local PCT (or equivalent organisation in other parts of the UK). Second, 38% of NAPP members were very optimistic about the future of their PPG, 46% were quite optimistic, 12% were a little optimistic and 3% were not optimistic at all.
This research is far from perfect and some of its shortcomings are described in the closing paragraphs. Yet it is valuable, we hope, in providing a deeper understanding of current PPG activity, future per-spectives and the attitudes of practices (primarily practice managers) towards PPGs. It should also stimulate and inform debate about the future devel-opments of PPGs and the support that they require. Next, we highlight three major issues.
The first issue is how practices could (or should) be encouraged to initiate a PPG. The obstacles identified by the research are clear, relating to lack of time and fears about the PPG being awkward and/or unrepre-sentative. So, what would lead practices to commit to establishing a PPG?
There is no national requirement for practices to have PPGs and it is not likely that this will be introduced in the coming years. Local schemes are increasingly common, however. Some practice-based commissioning groups (e.g. Principia in Nottingham) now require and incentivise their component prac-tices to establish PPGs, and it is clear, from NAPP’s experiences working with practice-based commission-ing groups groups, that this is proving effective. Yet the approach is not without its critics.
First, the PPGs themselves see Funding for practices as the lowest priority among ten factors that they were asked to rank in the members’ survey. They may feel that resources should be given to them (rather than the practices) so that they can communicate with other patients as effectively as possible. Second, PPGs worry that practices sometimes establish PPGs as a tick box exercise without being really committed to working with their patients in a new way. Finally, this approach may narrow the focus and remit of PPGs in a way that is unhelpful. Commissioning is clearly important but so are the other functions that PPGs undertake, notably around health promotion, information pro-vision and support to other patients.
Another possible motivation for practices to set up PPGs is that they are seen as an integral part of good general practice, possibly endorsed by processes of practice accreditation and professional revalidation. With the numbers of PPGs now well established at around four in ten English practices, we are probably still short of the level that will be required to persuade practices that PPGs are part of what might be de-scribed as a ‘cultural norm’. Yet, continued growth in line with recent trends could well see that point reached over the next decade. Professional leadership, as in the Growing Patient Participation campaign launched in June 2009, will accelerate that process.[2]
This ‘normalisation’ will also help PPGs who see their major challenge as securing the support and interest of more patients. If PPGs were present in most practices, levels of awareness about their role would rise and there would be more coverage in local, regional and national media. One can even imagine a situation where membership of the PPG carries a certain social status (as happens in some PPGs already). This may have the added benefit of widening the breadth of representation within PPGs.
The second major issue flowing from the research concerns the support that is available to PPGs. Only 25% of PPGs affiliated to NAPP reported receiving help from their PCT (or equivalent organisation),while PPGs see sharing of good practice, support from the PCT (or equivalent) and more networking opportunities as their top three priorities for future development. The requirements of World Class Com-missioning may encourage PCTs to respond to this need. Early evidence from NAPP’s work with the 11 project sites indicates that this approach can make a real difference, by boosting the profile of PPGs and providing mechanisms whereby they can learn from, and support, each other.
The third issue (or set of issues) relates to the central role of PPGs (as identified by practices with PPGs, practices without PPGs and NAPP-affiliated PPGs), namely providing the patient perspective. Interest-ingly, this needs to be set alongside two other findings:
(a) the fear of practices without PPGs that they will not be representative, and (b) the fact that practices without PPGs attach a low priority to PPGs under-taking research. Is there a way through this apparent mismatch between the recognised primary function of PPGs and the perceived weaknesses that make them ill-suited to that role?
This is an ongoing challenge since it is unlikely that any PPG committee will be able to reflect the diversity of the practice population. Its success in reflecting that wider view can be increased, however, by (a) networking effectively with local community and patient groups,(b) carrying out surveys in partnership with the prac-tice, including simply chatting to patients in the waiting room, (c) publicising the existence of the PPG and its role, and (d) using virtual models of engage-ment such as email networks and online discussions. The outcome may not be perfect but it is likely to add considerably to the practice’s own understanding of the patient perspective.
The methods used to generate these findings are somewhat messy, as a result of variations in questions and survey methods. The results, as presented here, also hide significant regional variations. Nonetheless, they provide fresh and important information in a number of areas that should be of interest to PPGs, practices, managers and policy makers. Equally, the survey results can inform the future research agenda, which can be taken up by academic institutions.
It would be particularly valuable if further work could be undertaken to assess and evaluate the costs and benefits associated with PPGs. Studies of this sort have only been undertaken on an extremely small scale, employing fairly simple techniques. It will be far from straightforward to calculate the gains from activities as diverse as patient education, influencing commissioning and advising the practice on the patient perspective. Nonetheless, further insights in this area are essential if we are to assess the full costs and benefits associated with the growing numbers of PPGs.
The research was partly funded by the Department of Health
Commissioned; not externally Peer Reviewed.
None.