International Exchange - (2005) Volume 13, Issue 3
Director, Division of Research, Department of Family and Community Medicine, School of Medicine, University of Alabama at Birmingham, Birmingham, AL, USA
Lesa L Woodby PhD MPH
Associate Professor, Division of Research and Associate Director for Education and Evaluation, Birmingham/ Atlanta Geriatric Research, Education, and Clinical Center (GRECC), Veterans Affairs Medical Center, Birmingham, AL, USA
Toya V Russell PhD MSPH
Assistant Professor, Division of Research
Tamela J Turner PhD MEd LPC
Director, Division of Predoctoral Education
Department of Family and Community Medicine, School of Medicine, University of Alabama at Birmingham, Birmingham, AL, USA
J Michael Hardin PhD
Professor, Department of Information Systems, Statistics, and Management Science, Culverhouse College of Commerce and Business Administration, University of Alabama, Tuscaloosa, AL, USA
T Michael Harrington MD
Chairman, Department of Family and Community Medicine, School of Medicine, University of Alabama at Birmingham, Birmingham, AL, USA
Received date: 29 April 2005; Accepted date: 10 August 2005
Background Although national clinical practice guidelines exist for treatment of tobacco use, little is known about the extent to which they are used in daily practice.Methods Nine hundred Alabama family physicians and internists were surveyed to measure self-reported knowledge and use of guideline elements as well as past participation and future interest in continuing medical education (CME).Results Of 215 physicians responding (24%), 67% reported they routinely ask patients about tobacco use. Most (81%) advise quitting, but less than half (45%) assess willingness to quit or assist with quit attempts, and fewer (41%) arrange follow-up. One in four (25%) had previously participated in CME; one in five (22%) were familiar with the guideline; four out of five (81%) were interested in CME on the subject.Conclusions Analysis revealed a correlation between experiencing CME and utilisation of guideline elements. In response, a CME programme and PDA-based protocol were developed to facilitate integration of the recommended 5-A intervention into daily practice.
continuing medical education, healthcare surveys, physician’s practice patterns, practice guideline, smoking cessation
Cigarette smoking has long been identified as one of the leading causes of preventable death, disability, and healthcare burden.[1,2] While public awareness about the dangers of tobacco use has increased dramatically since the first report by the United States Surgeon General was released 40 years ago, and statistics indicate that over 70% of people who smoke desire to quit, the national US adult smoking prevalence rate remains at 23%.[3,4]
National evidence-based clinical practice guidelines for the treatment of tobacco use and dependence have existed since 1996.[5,6] While little is known about the extent to which they are utilised in day-to-day practice, [7] study indicates that few are aware of the guideline or apply the recommendations consistently in practice.[8] Likewise, physician recommendation of nicotine replacement therapy (NRT) is also known to be varied and often low.[9,10] Alabama’s primary care physicians were surveyed to measure their self-reported knowledge of the guideline and use of key recommendations, as well as their interest in receiving continuing medical education (CME) on this topic.
Alabama’s current smoking prevalence rate is 24.4% for adults, and for smokeless tobacco the state ranks fourth in the nation. As in the US, tobacco use in Alabamatends to be associated with lower socioeconomic status and education. Among adults, 36.4% of people who smoke have annual incomes of less than $15 000, and 32.7% have less than a high school education.[11]
About half of Alabama’s 2250 primary care physicians (approximately 1400 family physicians and 850 internists) practise in rural areas. Many are the sole source of routine healthcare for the patients they serve.
Over half of all office visits in the US are to primary care practitioners, and the majority are for chronic illnesses (hypertension, diabetes, hyperlipidaemia and chronic obstructive pulmonary disease).[12]
Seven of ten people who smoke visit a physician each year. Most report that they value their physician’s advice regarding tobacco use, yet only half report ever being advised to quit.[13–16] Although few patients present with tobacco use as their primary complaint, and primary care physicians often address multiple ongoing problems, given that it exacerbates many common conditions it would seem important to address the issue within the context of routine office visits.
The 5-A model and potential for physicians to intervene
Using a simple algorithm (Figure 1), the national clinical practice guideline for the treatment of tobacco use and dependence suggests a brief, three-minute intervention based on the 5-A model of ask, advise, assess, assist, arrange (Box 1).[6] The first three As should be delivered to tobacco users at every visit. Discussions about tobacco use are more likely to take place during new patient visits than return visits, but because relapse and multiple quit attempts are the norm, repetition should occur at each visit.[10] For patients unwilling to quit, the 5-Rs should be implemented (Box 2).


For patients willing to quit, the two remaining As (‘assist’ and ‘arrange’ follow-up) should be implemented. A positive correlation has been found between patient cessation rates and inclusion of these two steps, yet they are implemented infrequently.[17,18] Scheduling constraints, lack of reimbursement, and lack of training in appropriate counselling methods have been cited as barriers to delivery of tobaccorelated counselling. Other barriers include a lack of belief in the effectiveness of tobacco use interventions, and lack of time during clinic visits compounded by the need to address multiple or complex problems.
Evidence indicates that even one minute of counselling can increase and sustain tobacco use cessation. [19–21] When combined with pharmacotherapy, behavioural therapies double patients’ likelihood of success.[5,6,22] The brief 5-A intervention can be integrated into routine care and is an important first step in positively affecting health outcomes for patients who use tobacco.[20,23]
Alabama Tobacco Free Families
At the time of this survey, the Alabama Tobacco Free Families (ATOFF) programme, funded by the National Cancer Institute, was being conducted at the University of Alabama at Birmingham Department of Family and Community Medicine. ATOFF’s primary goal was to reduce smoking prevalence among females of childbearing age and their families, especially those of low socioeconomic status. The programme included a provider education initiative. In preparation for the educational component, ATOFF assessed current versus best tobacco treatment practices among Alabama’s primary care physicians.
Pilot survey
Prior to the large-scale survey, a pilot study was conducted in partnership with the Alabama Practice Based Research Network (APBRN), a voluntary consortium of family physicians in academic and private practice throughout the state. A one-page survey instrument was developed following a review of the literature and consultation with national experts.[8,24–31] The survey’s 15 scaled questions addressed perceived tobacco use prevalence, knowledge and delivery of guideline (5-A) elements, delivery of counselling, information and pharmacotherapy, prior participation in CMEand interest in futureCME. Comments from the pilot study (98% response) guided refinement of the survey instrument, e.g. minor changes in wording and design.
Statewide survey
The statewide survey was faxed to 900 family physicians and internists, a representative sample (40%) of the 2250 primary care physicians (536 family physicians and 364 internists). In the US, family physicians and internists provide primarily the same services, although family physicians may also provide obstetric services and services for children. A cover letter from the president of each specialty’s state professional association requested participation. No monetary or other incentives were offered for completion. Second and third requests were faxed to non-responders; no telephone follow-up occurred.
A 24% response rate was achieved. While relatively low, the responses were consistent with those given in the pilot, and the rate was consistent with similar surveys conducted among physician populations using similar methods (survey by fax), but was lower than the average return for mailed surveys.[32–34] Research indicates that surveys by fax are preferred by physicians and, even then, the response rates vary widely (27% to 58%).[32–33]More family physicians responded (146/536, 27%) than internists (69/364, 19%), perhaps due to the project’s departmental affiliation.
The 5-As
Overall, 67% of respondents reported that they always ask patients if they use tobacco, family physicians much less than internists (62% versus 78%). A chi-square calculated on the significant difference between specialties was 5.57; P = 0.018. Family physicians were also slightly less likely to advise quitting than internists (80% versus 84%), a chi-square difference of 0.48; P = 0.49. Fewer than half of respondents always assess tobacco users’ willingness to quit, family physicians slightly less than internists (43% versus 48%). A chisquare test of differences was 0.41; P = 0.52.
Approximately one-half of physicians reported that they always assist tobacco users with quit attempts: 50%, family physicians; 55%, internists, chi-square test 0.42; P = 0.52. Fewer respondents (41%) said they always arrange follow-up for patients willing to quit, family physicians more frequently than internists (44% versus 35%), chi-square analysis 1.59; P = 0.21.
Counselling, information and pharmacotherapy
Of physicians who reported that they assist patients with quit attempts, 47% stated they always provide counselling, with family physicians and internists equally likely to do so (47% and 46%). A chi-square test of the difference was 0.0007; P = 0.98.
Very few physicians (18%) reported they always provide information on quitting, such as pamphlets, videos or online resources. Family physicians were more likely to do so than internists (20% and 15%). The chi-square analysis was 0.87; P = 0.35.
One-quarter (27%) stated they always recommend pharmacotherapy for patients willing to quit, with internists more likely to prescribe than family physicians (30% versus 22%). The difference between responses was significant: chi-square 6.97; P < 0.008. Bupropion was most commonly recommended, followed by nicotine patches, gum, inhaler, and nasal spray. Nicotine lozenges were not available at the time of the survey.
Knowledge of the guideline and CME
Only one in five physicians (22% each specialty) reported having knowledge of the guideline. Similarly, only 25% (29% family physicians, 16% internists) reported previous participation in a CME programme on tobacco cessation. More than two-thirds of physicians surveyed (81% each specialty) were interested and willing to participate in such a programme.
Logistic regression analysis
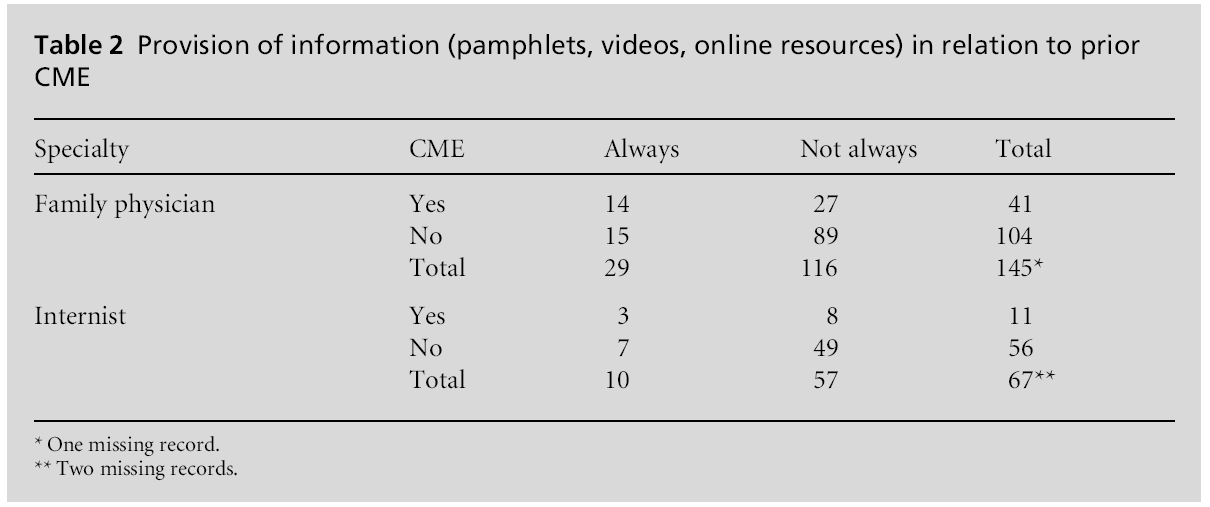
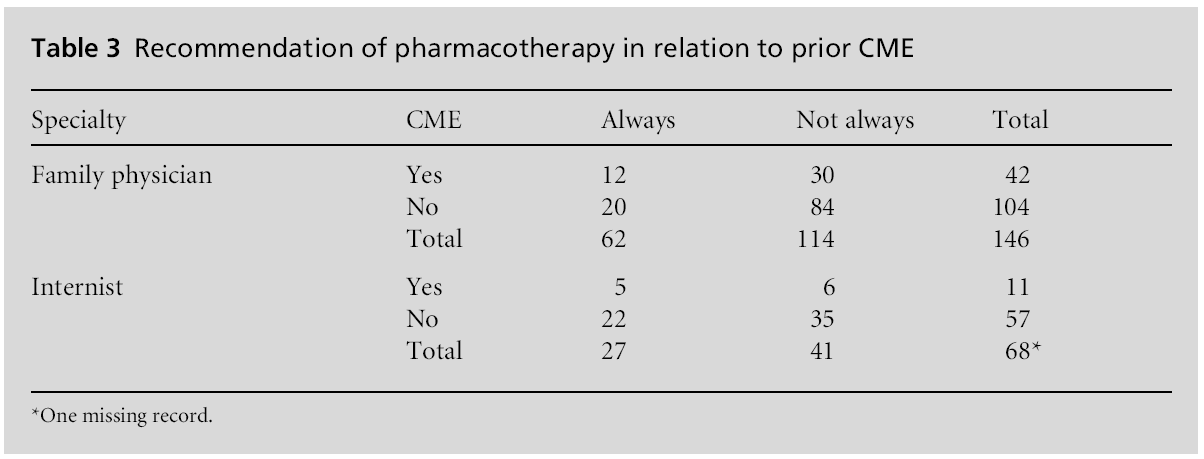
A logistic regression analysis was performed to explore the significance of prior participation in CME in relation to the frequency of 5-A delivery as a determinant of responses between specialties. Three questions contained significant variables: how often physicians ask patients if they use tobacco (Table 1), how often they provide information (Table 2), and how often they provide pharmacotherapy (Table 3).
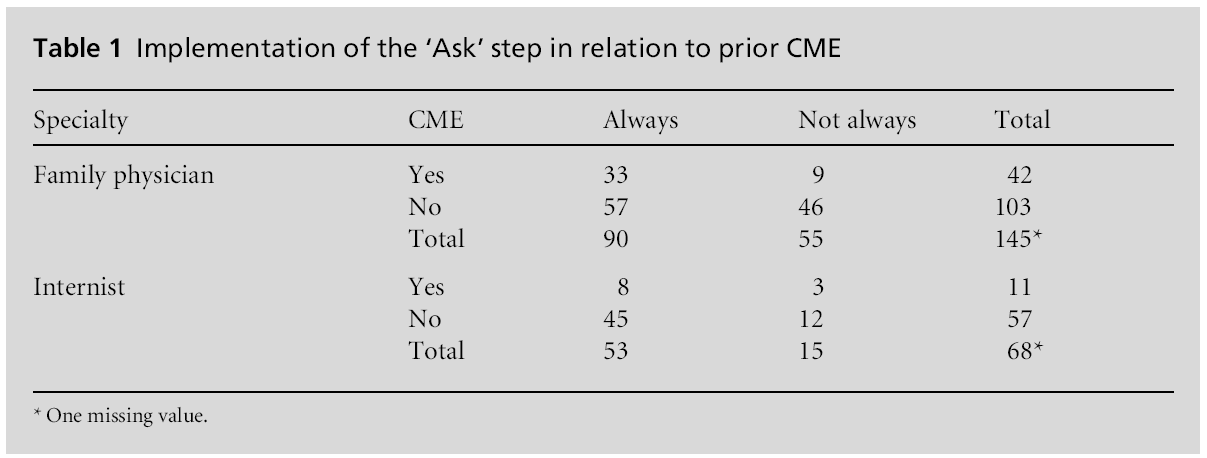
Physicians who had previously participated in a CME programme were twice as likely to always ask if their patients use tobacco and to provide information, such as pamphlets, videos, or online resources. Family physicians were 60% less likely to always ask if their patients used tobacco. The logistic regression equation (Table 1) was 1.16–0.88 specialty+ 0.80 CME. The odds ratio for specialty was 0.42 and for CME, 2.23.
Physicians who had previously participated in a CME programme were five times more likely to provide information on quitting than those who had not. The logistic regression equation (Table 2) was –1.16 + 1.59 CME. The odds ratio for CME was 4.92. The variable specialty was not significant.
Logistic regression analysis revealed that family physicians were 60% less likely than internists to provide pharmacotherapy. The logistic regression equation (Table 3) was –0.49 – 0.92 specialty. The odds ratio for specialty was 0.399. The variable CME was not significant. The analyses indicate a positive relationship between participation in CME programmes and screening for tobacco use and provision of supplemental information to patients.
This survey revealed a low level of knowledge and utilisation of the national clinical practice guideline on the treatment of tobacco use and dependence, and a strong interest inCMEon this topic among Alabama’s primary care physicians. While most routinely ask patients if they smoke, and many advise smokers to quit, few assess patients’ willingness to quit. Furthermore, patients who are motivated to quit only receive assistance about half the time, representing missed opportunities to move patients to action. Counselling is frequently provided, but information and pharmacotherapy are not, which is consistent with previous findings. Because both elements are recommended to maximise tobacco use cessation, half the support that patients need is not being administered.
Limitations
Because of limitations in the nature and size of the sample, findings from this survey may not be generalisable to a larger population of physicians by specialty or geographic distribution. Although the response rate was comparable to that of other surveys faxed to physicians, one could argue that responders would be more aware and active in smoking cessation than non-responders, causing the results to be an overestimate of activity. Respondents’ tobacco use status was not assessed, a factor known to affect the frequency and type of intervention given to patients who use tobacco.[35] Because no sociodemographic information was solicited, there was no way to discern if respondents were similar to, or different from, nonrespondents. While the survey was limited to one page for ease of completion, presentation of the scale may have influenced responses in that the desired response (‘always’) was easily discernible. Physicians were not asked if they treated patients who smoke differently at initial visit compared to return visits, perhaps influencing interpretation of questions related to frequency of delivery. Finally, self-reports are not necessarily reliable, even among physicians.[17]
Dissemination of the revised 1996 guideline in 2000 was carried out through publication of articles in scholarly and specialty-specific journals, which are not always read by primary care clinicians. Distribution of the guideline also occurred at national and international meetings targeted to smoking cessation providers and researchers, and was posted to government websites and those created for the purpose of educating the public about the dangers of tobacco use – none functions that would commonly reach community-based physicians. Despite widespread dissemination, this survey suggested that the guideline had not reached many primary care physicians at the community level and that guideline recommendations were not being consistently implemented in such practices. Further efforts to educate physicians in how to integrate guideline-recommended intervention strategies into daily practice appeared to be warranted.
Two significant steps were taken. First, ATOFF created a CME programme using academic detailing as the educational strategy, and addressing known barriers to implementation in practice.[25,36,37] Training in delivery of a brief 5-A intervention was conducted at state professional conferences, as well as family medicine residency programmes and individual practices. The programme was also added to the curriculum for medical students rotating through the University of Alabama’s Family Medicine clerkship, significant because few medical school curricula currently include tobacco cessation training.[38] Training was also delivered to non-physician healthcare providers and organistions, targeting those supporting primary care.[28] To further aid physicians in implementing the ‘assist’ and ‘arrange’ steps, ATOFF produced a series of patient education brochures which were made available free of charge to Alabama physicians and other healthcare providers.
Second, the APBRN developed a PDA-based assessment and counselling programme which guides physicians through a brief 5-A intervention at the point of care. The programme includes ‘value added’ features (e.g. automatic Fagerstrom score calculation, behaviour modification tips, the 5-Rs) which support personalisation of each intervention – a factor known to be important to patient compliance.[39]
Opportunities abound for primary care physicians to address tobacco use cessation with patients during office visits. Efforts are needed to help physicians incorporate guideline recommendations into routine care, with special attention to the challenges of daily practice.[40] An examination of current versus best practices is a recommended first step.
Appreciation is extended to the physician members of the Alabama Practice Based Research Network, to the state primary care professional associations for their assistance with the survey, and to the experts who assisted with survey preparation. Special thanks to JM White and Billie Anderson for their assistance in preparing this manuscript.
None.