Research Paper - (2013) Volume 21, Issue 3
James E Rohrer PhD1, Michael L Grover DO2 and Carolyn C Moats MD3
2Assistant Professor, Vice Chair-Research
3Instructor, Department of Family Medicine, Mayo Clinic, Scottsdale, AZ, USA
Corresponding Author:
James E Rohrer PhD
Department of Family Medicine
Mayo Clinic
200 First St. SW Rochester MN 55905 USA
Email: rohrer.james@mayo.edu
Received date: 1 February 2013; Accepted date: 10 April 2013
BackgroundQuality improvement investigators working in field settings, who typically are not trained in epidemiological methods, may not consider all three elements of the epidemiologic triad (person, place and time) when planning their projects. AimTo demonstrate how the epidemiological triad can guide analysis for quality assessment. Predictors of antibiotic use in primary care were analysed to illustrate the approach. MethodsThis study was a secondary analysis of data previously collected from medical records and a provider survey. A convenience sample of 467 family medicine patients treated in two clinic sites for acute respiratory tract infectionswas analysed by locating quality variation in person, place and time Independent variables included patient age, date of clinic visit, and clinic site. The outcome measure was antibiotic prescription (yes or no). ResultsAntibiotics were prescribed for 69.2% of patients in the sample. Age group was not related to antibiotic prescribing. Prescription was related to time (P = 0.0344) and clinic site (P = 0.0001) in univariate tests. However, only site was independently related to antibiotic prescription (odds ratio = 0.47, confidence interval = 0.30 to 0.73, P = 0.0008). ConclusionThe epidemiological triad assisted in guiding further post hoc analysis of predictors of antibiotic prescriptions. Further investigations of this quality indicator can be directed at exploring site differences and testing interventions. Studies of other quality indicators in primary care can employ the triad to guide the analysis.
Keywords
acute respiratory tract infections, antibiotic prescriptions, epidemiological triad, managerial epidemiology, outbreak investigations
Introduction
Investigations of quality in primary care require analysis of variations in quality indicators and testing for associations with predictor variables. Analysis of existing data, such as those found in electronic medical records, is an important first step. Although the range of choices for analytical approaches can be daunting, adjusting for possible confounders using regression analysis is important. Adopting a perspective drawn from clinical epidemiology and investigations of disease outbreaks can be helpful. The epidemiological triad, as applied to studies of medical care quality, directs investigators to locate variation in person, place and time.[1–3] Some publications address all three elements of the triad. However, quality improvement investigators working in field settings, who typically are not trained in epidemiological methods, may not consider all three elements when planning their projects.
The purpose of this study was to demonstrate the use of the triad in quality assessment by applying it to analysis of one particular quality indicator: antibiotic prescriptions in family medicine for acute respiratory tract infections (ARTI). A limited number of recent studies has treated this as a quality indicator, searched for root causes or demonstrated successful strategies for improvement.[4–10] The triad is a simple yet comprehensive model for guiding investigations. Our goal is for practitioners to consider using the triad in their own studies of variation in clinical quality indicators.
Methods
This study demonstration employs a set of data previously collected, analysed and reported.[4,10] The tables and figures included in this report, however, have not been published or reported elsewhere. Eligibility for this observational study was limited to adult patients with ARTI. Data were collected during the time frame 16 December 2009 to 5 March 2010. Two methods were employed. In one clinic, data were extracted retrospectively from the electronic medical record (Clinic A, n = 187). In the other clinic, data were collected prospectively (Clinic B, n = 280). The prospective approach in Clinic B was used so that explanations for prescriptions could be obtained from providers. The two data sets were pooled for statistical analysis.
No patient identifiers were supplied to the data analyst. Our Institutional Review Board has determined that retrospective studies of de-identified data for quality improvement purposes are not subject to human subjects review.
The dependent variable was an antibiotic prescription (scored yes or no). Independent variables were clinic location, employee status (versus not an employee), patient age, patient gender and day of week.
Univariate tests were performed using chi-square tests. Variation over time was analysed graphically. Multiple logistic regression analysis was employed to identify independent predictors of antibiotic prescription. Epi-Info, a free-ware package from the Centers for Disease Control and Prevention, was used for statistical analysis.
Results
A longitudinal analysis of antibiotic prescriptions is presented in Figure 1. Clinic days in which the number of ARTI cases was zero were omitted from the chart. The daily rate of prescriptions can be seen to show a downward trend after 1 February. In addition, the standard deviation increased from 17.3 to 18.7.
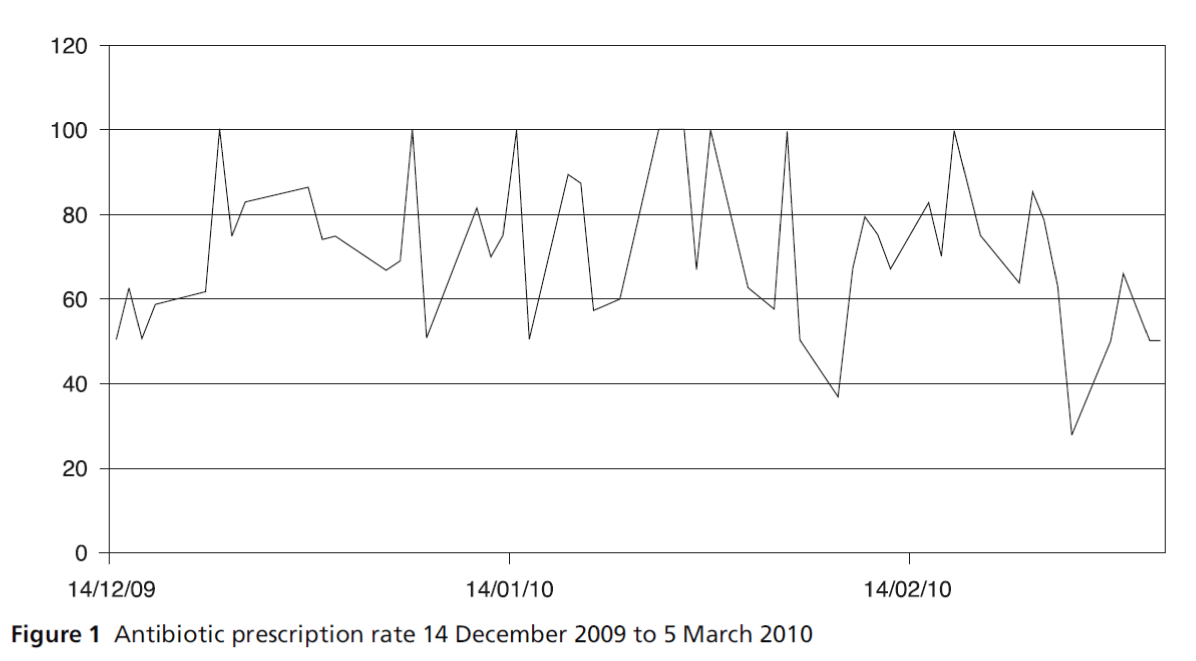
Figure 1: Antibiotic prescription rate 14 December 2009 to 5 March 2010
Results of univariate tests are shown in Table 1. Antibiotics were prescribed for 69.2% of patients in the sample. Age group was not related to prescribing antibiotics. Prescription was related to time (P = 0.0344) and clinic site (P = 0.0001). However, as can be seen in Table 2, only site was independently related to antibiotic prescription [odds ratio (OR) = 0.47, confidence interval (CI) = 0.30–0.73, P = 0.0008]. The univariate association between time and prescription was due to the concentration of Clinic A cases in the earlier period. Antibiotic prescription rates were higher in Clinic A.
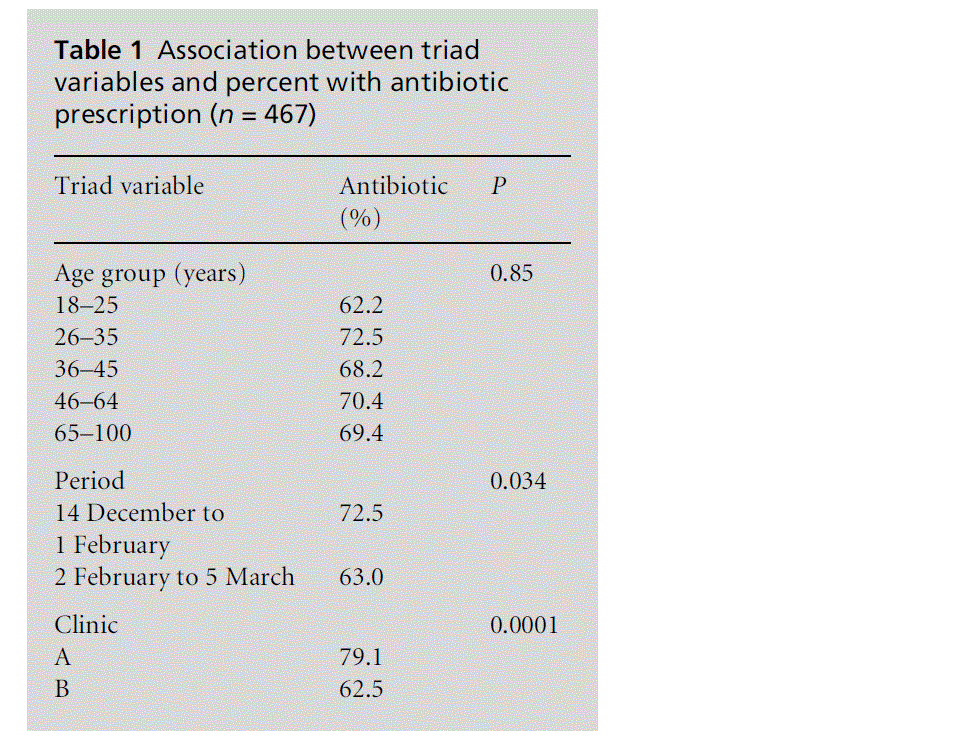
Table 1: Association between triad variables and percent with antibiotic prescription (n = 467)
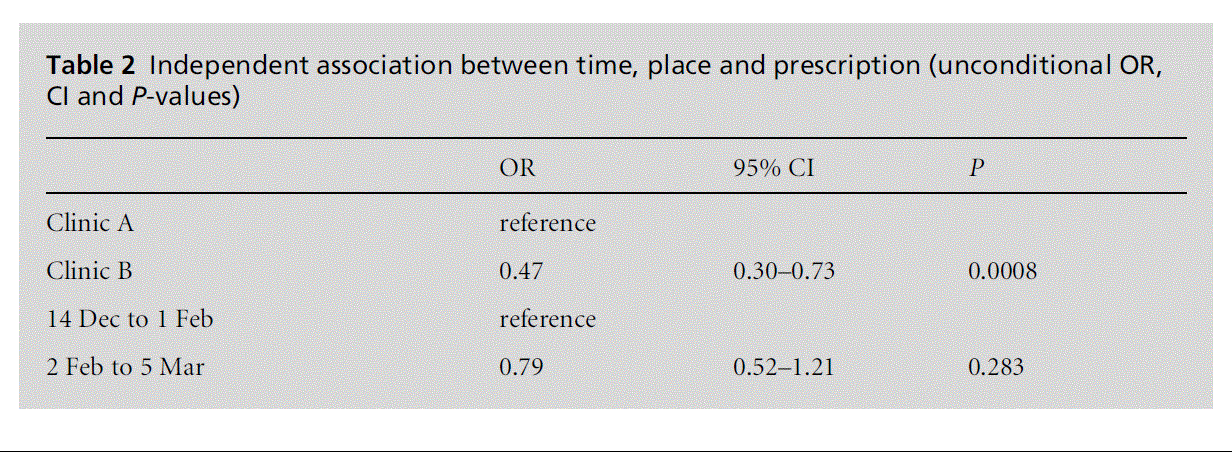
Table 2: Independent association between time, place and prescription (unconditional OR, CI and P-values)
Discussion
This retrospective study of antibiotic prescriptions for ARTI patients seen in family medicine clinics is an example of managerial epidemiology in that it applies epidemiological methods to a managerial concern.[11] The results show that the epidemiological triad can be useful for guiding the analysis clinical quality indicators. Investigation of personal characteristics (clinical and demographic variables) is second-nature in quality assessment. Control charts showing variation over time may or may not be included. Site comparisons may be involved. Deliberate inclusion of all three dimensions may not be part of the planning process, however.
Our analysis of antibiotic prescriptions revealed that in univariate tests both time and clinic site were associated with prescriptions. The association with clinic site was not surprising because prescribing rates are affected by physicians’ desires to satisfy anticipated patient expectations[5] and willingness to be firm with patients probably varies among physicians. The apparent association with time proved to be an artefact of the association between time and clinic site. This helps us understand the sources of variation in our data. We hasten to add, however, that these data were cross-sectional and causality cannot be inferred. The association between clinic site and prescribing might not be causal. We are particularly aware of the possibility of a methods effect: data were collected retrospectively in the clinic where rates were higher. It is possible that prospective data collection in Clinic B alerted the staff and caused them to change their prescribing behaviour. If this proves to be true, then we regard it as useful information, because it suggests an intervention.[10] Perhaps prospective monitoring of prescribing is sufficient to achieve improvements in quality. Additional studies are needed to confirm this hypothesis.
Published epidemiological studies may or may not include all three dimensions of the triad. We offer two examples to illustrate the point. In Grijalva et al[7] evaluation of trends in antibiotic prescribing for ARTI used all three aspects of the epidemiologic triad. The authors analysed trends from 1995 to 2006 in two-year intervals by query of the National Ambulatory Medical Care Survey and National Hospital Ambulatory Medical Care Survey databases. The two-year intervals provided a time element, one leg of the triad. ‘Person’ criteria were utilised as independent predictors of the dependent outcome of antibiotic prescribing, for example, by categorising patients as children under 5 years of age and those aged 5 years and greater. Although rates in antibiotic prescribing decreased in both groups, rates were shown to be significantly greater in children under 5 years of age (41% decrease versus 24%) and appeared to be related to a 33% decrease in rates of otitis media office visits (personrelated variable of final diagnosis). Place was analysed by categorisation of location of the patient encounter – emergency department (ED), hospital-based outpatient clinic or physician practice. Change in rates were seen over time only in physician practices (63% 1995–1996 to 52% 2005–2006 for patients 5 years and greater; P = 0.02), whereas no significant changes were seen in rates over time in hospital clinics or EDs. Given the objective of monitoring trends in a national sample, prescribing rates were not described at the practice group or individual prescriber level.
The study described above contrasts with that reported by Vinnard et al6 who examined the effect of two types of interventions on antimicrobial prescribing for acute bronchitis patients (i.e. an ‘intensive’ intervention of provider academic detailing, a ‘mild’ patient mailing intervention and a control group with no interventions). Time was minimally addressed with pre- and post-intervention data and no trend lines. Variation among patients according to personal characteristics was not reported. Instead of sorting data by practice site, the authors focused on analysing differences among individual providers. Provider prescribing rates were the outcome of interest and were examined in terms of not only which of the interventions had been assigned to each group but by practice site and individually at a provider level, both pre- and post-intervention. Wide variability was seen in baseline antibiotic prescribing behaviours, both for providers, and those in the control and intervention groups. This knowledge was utilised as justification to focus the most intensive interventions toward those providers with the highest rates of use, who worked at intervention practice sites.
In Ong et al,5 evaluation of antibiotic prescribing for bronchitis and upper respiratory infection in the ED setting utilised only the person criteria of the epidemiologic triad.
The authors analysed whether physicians were more likely to prescribe antibiotics when they believed their patients expected them, and whether those beliefs were actually correct, by interviewing both the patient and the physician separately. Physicians were more likely to prescribe antibiotics to patients who they believed expected them; physicians, however, only correctly identified those patients about 25% of the time. Receiving an antibiotic was associated with the physician’s perception of the patient’s expectations (OR = 5.3; 95% CI = 2.9–9.6), but paradoxically was not associated with the patient’s actual expectation of antibiotics (OR = 1.4; 95% CI = 0.8–2.2).
‘Person’ criteria might apply to both the patients and the physicians as both were studied; physicians were interviewed about factors that influenced their medical decision making, including their perceptions of their patient’s expectations of the visit. Patients were interviewed prior to seeing the physician, after seeing the physician and two weeks after discharge in a telephone interview. Prior to seeing the physician, patients were asked what they expected in terms of medical treatment during the visit, i.e. laboratory tests, X-ray, prescriptions and hospitalisation, and whether they believed that any medications would be important in shortening their illness. The interview conducted after seeing the physician included questions about whether they received an antibiotic prescription, whether they had a better understanding of their illness and quantified their satisfaction with the ED visit. Trends in prescribing were also collected for attending versus resident physicians, showing attending more likely to prescribe an antibiotic than a resident physician. Results of antibiotic prescribing were analysed by multiple patient characteristics of symptoms (i.e. cough), clinical characteristics (i.e. oxygen saturation) and the condition of being insured versus not being insured. Those patients with insurance were less likely to receive an antibiotic; 21% of insured patients versus 38% of uninsured patients received an antibiotic prescription (OR = 0.4; 95% CI = 0.3–0.7).
‘Place’ was ten urban academic EDs. The authors did not report statistics of the individual EDs. This does not fulfil the ‘place’ criteria of the epidemiologic triad. ‘Time’ criteria considerations included having two separate two-week enrollment periods in different seasons, winter 1999–2000 and summer 2000 to reduce seasonal variations in treatment. The data on these two enrollment periods was presented but did not include enough time points to allow for analysis of patterns.
We do not intend to suggest that published epidemiological studies of quality improvement are not of high quality unless they thoroughly examine variations in person, place and time. However, practitioners in field settings who are planning projects might be advised to incorporate the elements of the triad before beginning.We say this because the triad is a time-honoured rubric long found to be useful in epidemiology. Quality improvement analysts who are trained in fields other than epidemiology may still find it to be a useful paradigm.
Clustering effects are often ignored in quality assessment analyses. A strength of our study is that the two sites were treated differently. However, when multiple sites are included in a study without any obvious differences among sites, potential clustering effects are often ignored. An appropriate analysis approach for a study with several clusters could be a random effects model with patient-level characteristics included as fixed effects and clinical sites/clusters included as a random effect. Such an analysis would yield separate estimates for the amount of variability of the outcome on the patient level and on the cluster level.
A full epidemiological investigation of variations in antibiotic prescriptions for ARTI might include age of the physician, reimbursement system and prescribing practices related to place. However, investigations limited to a single medical care organisation do not require controlling for as many variables as would be necessary in larger multisite studies.
The data presented in this paper are too limited to serve as a stand-alone research study of variations in prescribing practices. However, preliminary quality improvement studies in field situations should be conducted to establish baseline data and assess whether fuller investigations are necessary. These will of necessity rely on data that are readily available from electronic medical records rather than primary data collection. Therefore, an example such as this intended for didactic purposes can be expected to use limited data for illustrative purposes.
Post-hoc data-driven selection of variables for analysis can be misleading. However, different types of epidemiological investigations are subject to different expectations in regard to the degree of rigor. Managerial epidemiology is more similar to outbreak investigations than to research epidemiology. As described by the Centers for Disease Control and Prevention, outbreak investigations may refine hypotheses and include additional variables midway through an investigation.[11]
The findings from our current analysis may have limited generalisability, because they represent results from one practice and only include a small number of independent variables. Clinical information was not analysed in this example. We note, however, that prescribing rates were shown not to be related to risk factors associated with complications in a previous report from these data.[4] Despite the limitations of the study, we believe using the epidemiological triad is potentially useful to other investigators because it offers a simple yet comprehensive framework for guiding the analysis of variations in quality indicators.
Conclusions
The epidemiological triad is a simple yet useful rubric for guiding investigations of clinical quality. In this example, the triad assisted in guiding analysis of predictors of antibiotic prescriptions. Further investigations of this quality indicator can be directed at exploring site differences and testing interventions. Studies of other quality indicators in primary care can employ the triad to guide their analyses.
Funding
Unfunded.
Ethical Approval
The Institutional Review Board has determined that retrospective studies of de-identified data for quality improvement purposes are not subject to human subjects review.
Peer Review
Not commissioned; externally Peer Reviewed.
Conflicts of Interest
None.